Novel drug that opens the lungs’ airways - an effective treatment for asthma patients
- Scientists identify a compound that relaxes airway smooth muscle cells to treat asthma
- The drug called TSG12 has been developed from a protein called metallothionein-2 or MT-2 that relaxes smooth muscle cells in asthmatic lung tissue
- TSG12 is non-toxic and more-effective than bronchodilators currently used to treat asthma
"It is not a cure, but I think this treatment will give people a lot of hope," said Luis Ulloa, a lead author, and immunologist at Rutgers New Jersey Medical School. "There are a growing number of patients with no alternative because the current treatments either have critical side effects or aren’t working. We hope this will give patients a better option."
Study
The study scientists discovered that a particular protein called metallothionein-2 (MT-2) present in asthmatic lung tissues relaxes airway smooth muscle cells and opens the airways, thus allowing asthma patients to breathe.Ulloa and his collaborators also found other connections between MT-2 and asthma by transmitting short electrical pulses into mice through electro-acupuncture needles and discovered that
- MT-2 was over 50 percent lower in asthmatic lung tissue
- Mice without the MT-2 protein were two times more susceptible to asthma. When they treated the mice with MT-2, the protein improved breathing of asthmatic mice
Current drugs in the market have critical side effects, depress the immune system and increase the risk of secondary infections, provide inadequate relief for about one-third of those who have asthma, and over time patients could develop resistance to these drugs.
"We found that the TSG12 used in the study is both non-toxic and more effective in reducing pulmonary resistance and could be a promising therapeutic approach for treating asthma without losing their effectiveness over time. The next step would be clinical trials" Ulloa said.
Asthma
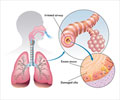
Asthma is a common, chronic respiratory disease. Worldwide, there are over 300 million and 65 million people affected by asthma and COPD respectively. In the United States alone, there are over 40 million people with asthma and another 11 million people suffering from COPD. In asthma and other respiratory illnesses, the airways or bronchial tubes that are responsible for air to flow into and out of the lungs get inflamed. When a person is exposed to an asthma trigger, the airways get even more swollen and the smooth muscle cells or SMCs around the airways contract or tighten. This makes it difficult for air to move in and out of the lungs and the person suffers from recurrent attacks of breathlessness, coughing, wheezing and chest tightness that varies in intensity and frequency from person to person.- L.-M. Yin el al., "Transgelin-2 as a therapeutic target for asthmatic pulmonary resistance," Science Translational Medicine (2018).