Local antibiotic medications are being over-prescribed for acute conjunctivitis in the United States, suggested a study.
- Local antibiotic preparations are being over-prescribed for acute conjunctivitis, revealed a study in the United States
- The lack of diagnostic techniques and the expectations from the patients could be partly responsible
- Physicians should be encouraged to adopt evidence-based practices for acute conjunctivitis
TOP INSIGHT
Local antibiotics that are misused for non-bacterial conjunctivitis increase the risk of side effects and drug resistance, as well as the cost of treatment.
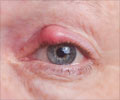
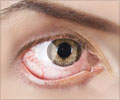
In their study, the scientists found that antibiotic eye preparations were being over-prescribed for acute conjunctivitis. Conjunctivitis is also called pink eye or sore eyes. The eyes appear reddened, with itchiness and discharge. Though bacteria can cause conjunctivitis, viruses and allergies are often more common causes.
The authors of the study checked out prescriptions for acute conjunctivitis filled out by 3,40, 372 patients in the United States between the years 2001 through 2014. They found that:
- Around 58% patients filled one or more local antibiotic prescriptions within 14 days of the diagnosis. This appears to be inappropriate, since most cases of acute conjunctivitis are either due to viral infection or an allergy. Even mild bacterial infections may not require an antibiotic.
- One out of every 5 among these received an antibiotic-steroid combination. Such combinations should be avoided in acute conjunctivitis since steroids can actually prolong the duration of or worsen an infection.
- Patients at a higher risk for developing serious eye infection following acute conjunctivitis like those with HIV or contact lens users. filled antibiotic prescription at a similar frequency compared to those who were not at a higher risk. On the other hand, education and affluence appeared to play a role in filling antibiotic prescriptions, with the more educated and the affluent more likely to fill antibiotic prescriptions compared to the less affluent or less educated.
- The patients were more likely to fill an antibiotic prescription if they were first seen by an urgent care physician, internist, pediatrician or family practitioner as compared to an ophthalmologist.
Reference:
- Shekhawat NS, Shtein RM, Blachley TS, Stein JD. Antibiotic Prescription Fills for Acute Conjunctivitis among Enrollees in a Large United States Managed Care Network. DOI: http://dx.doi.org/10.1016/j.ophtha.2017.04.034
 MEDINDIA
MEDINDIA


 Email
Email