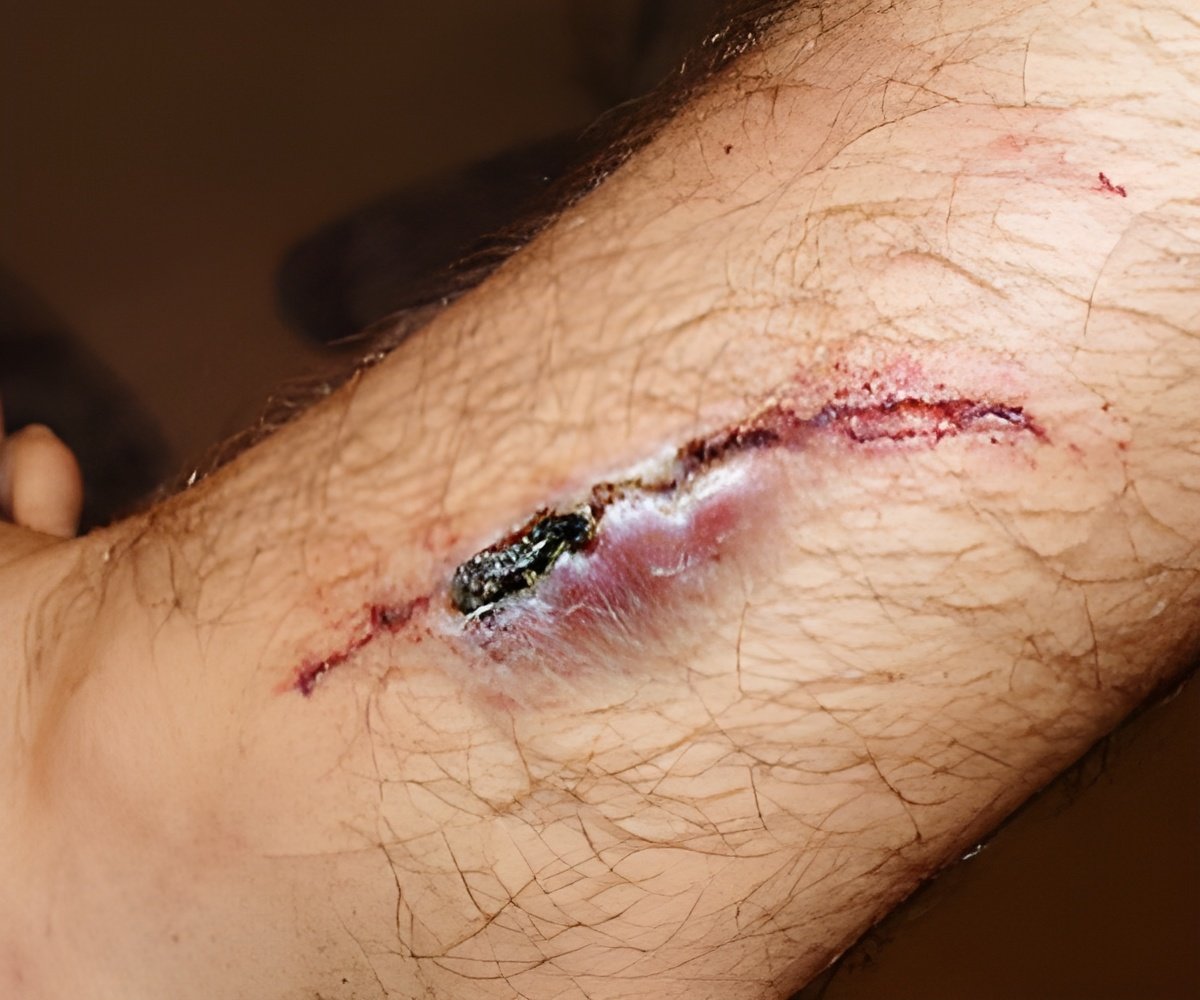
Septic shock comprises a subset of sepsis in which underlying circulatory and cellular metabolism abnormalities are severe enough to increase the risk of death.
TOP INSIGHT
Sepsis is a life-threatening organ dysfunction caused by a dysregulated host response to infection.
The investigators found that sepsis in mice bred to be deficient in SHARPIN resulted in enhanced levels of interleukins 1β and 18 and active caspase 1, as well as shortened survival. Treatment with a caspase 1 inhibitor reversed these effects by reducing levels of interleukins 1β and 18, decreasing cell death in the spleen, and prolonging survival.
The investigators also reported for the first time that this mechanism may be relevant to human sepsis. "We found a decline in SHARPIN levels in septic patients correlating with enhanced activation of caspase 1 in circulating mononuclear cells and an increase of interleukin1β/18 in the plasma," noted Dr. Schaefer. "Our findings suggest that using pharmacological caspase 1 inhibitors could be beneficial in septic patients with low SHARPIN levels and these therapies may be more efficient than other anti-inflammatory therapies."
A recent Task Force convened by the Society of Critical Care Medicine and the European Society of Intensive Care Medicine (JAMA 2016;315:801) define sepsis as "a life-threatening organ dysfunction caused by a dysregulated host response to infection." Septic shock comprises a subset of sepsis in which underlying circulatory and cellular metabolism abnormalities are severe enough to substantially increase the risk of death. Symptoms of sepsis include changes in body temperature, rapid heart rate, and rapid breathing. Other indicators are reduced urine output, changes in mental status, breathing difficulty, abdominal pain, and low platelet count.
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email





