The prevalence of food allergy has been increasing in the U.S affecting 8% of children adding an economic burden of $24.8 billion annually.

TOP INSIGHT
African American children are allergic to wheat, Latinos to corn, fish and shellfish while peanuts, tree nuts were a common allergen to many.
"Our goal was to characterize the food allergy related outcomes in these children and to identify any disparities in health care usage among African American, Latino and white children with food allergy."
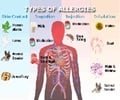
Food allergy is an immune system reaction that occurs soon after eating a certain food. Even a tiny amount of the food individuals are allergic to can trigger signs and symptoms, such as digestive problems, hives, breathing problems or anaphylaxis (a severe, potentially fatal allergic reaction).
Food allergy is major public health concern affecting eight percent of children in the U.S. with an estimated economic burden of $24.8 billion annually.
"It has been well documented that the prevalence of food allergy has been increasing in children in the U.S., but little data and research exists about its frequency, severity and outcomes among minority race and ethnicities in the U.S.," said Mahdavinia.
The study included 817 children in all and was composed of 35 percent African Americans (285 children), 12 percent Latino (99 children), and 53 percent non-Hispanic white children (433 children).
"We found African American children had a significantly higher rate of wheat allergy than did white children," said Mahdavinia. "Wheat-based bread is a staple in the U.S. and consumed on a daily basis in most U.S. households with an average consumption of more than 130 pounds per person per year.
Wheat allergy can be a significant financial burden, especially for low-income families," said Mahdavinia. "The higher rate of wheat allergy among African American children could potentially explain the higher rates of anaphylaxis, which is a severe allergic reaction that requires immediate care, and the emergency room visits observed in this population."
Latino children had significantly higher odds of allergy to corn, fish and shellfish, but a similar rate of asthma compared to non-Hispanic white children. The rate of corn allergy in Latinos could due to corn being a major food staple in Mexican and Hispanic families.
The study also found that compared with whites, African American and Latino children received less follow-up care for food allergy from an allergy specialist and had higher rates of food allergy related anaphylaxis and emergency room visits.
In this study, 55 percent of African American, 18 percent of Latino and 11 percent of white children were covered by Medicaid, indicating lower income rates among the African American families participating in the study.
Low income children incur higher costs for emergency room visits and hospitalization and spend less on specialty care. Shorter follow-up duration can negatively affect food allergy outcomes and can increase rate of death.
Peanut was the most common food allergen in all three groups. The only allergen more common among white children than African American and Latino children was tree nut. Tree nut allergies are distinct from peanut allergy because peanuts are legumes, whereas a tree nut is a hard-shelled fruit.
"A major concern is that African American and Hispanic children had significantly higher rates of food-induced anaphylaxis than White children. Furthermore, African American and Hispanic children also had higher odds of emergency room visits for food allergy related reactions compared to White children," said Mahdavinia.
"The three centers evaluated their patient population separately, but when we pooled the data together we saw the striking similarity of the findings among the centers, which confirmed our initial suspicion that food allergies present differently in various races. This is an important issue to make pediatricians and allergist aware of so they can look for the relevant allergies in each of the various races," said Dr. Amal Assa'ad, study co-author and allergy and immunology expert at Cincinnati Children's Hospital Medical Center.
"We found a difference in the insurance coverage among the various races, which may impact access to care and adherence to follow up visits and avoidance measures," added Assa'ad.
"We need to conduct further research to identify food allergy and food sensitivities among all races and ethnicities so we can develop culturally-sensitive and effective educational programs to improve food allergy outcomes for all children," said Mahdavinia.
"It is critically important for us to understand food allergy in children of different races and ethnicities, so we can improve management for all children," said Dr. Ruchi Gupta, senior author of the study and pediatrician and researcher at Ann & Robert H. Lurie Children's Hospital of Chicago and Associate Professor of Pediatrics and Medicine at Northwestern University Feinberg School of Medicine.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email