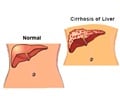
Novel techniques can identify severe infection (sepsis) hours after onset from early changes in liver function and this can be helpful in treating patients who are critically ill.
In this study, the authors from Austria, Germany, and the UK, led by Peter Recknagel from Jena University Hospital in Germany, used experimental laboratory work in cell cultures, genetically modified mice and rats, and studies carried out in critically ill patients to shed light on the mechanisms behind severe sepsis.
They found that in animal models, liver dysfunction is an early sign of sepsis and that a process known as PI3K signalling (which is involved in several immune processes) plays a crucial role in the development of liver dysfunction. The authors also found that all aspects of detoxification by the liver are affected during sepsis, a finding which suggests that clinical outcomes are linked to the severity of these liver changes.
The clinical information included in the study from 48 patients with severe sepsis also supports the finding from the animal models and suggests that liver function tests might help in the early diagnosis of sepsis and also provide information about possible clinical outcomes. As many medicines are broken down in the liver, these findings suggest that giving certain drugs to patients with severe sepsis may further damage the liver.
The authors explain their findings: "Liver dysfunction is an early and commonplace event in the rat model of sepsis studied here; PI3K signalling seems to play a crucial role. All aspects of hepatic biotransformation are affected, with severity relating to subsequent prognosis."
They continue: "Detected changes significantly precede conventional markers and are reflected by early alterations in plasma bile acids."
Advertisement
In an accompanying Perspective, John Marshall, a critical care expert from the University of Toronto (uninvolved in the study), says: "The hybrid translational model embodied in the work reported here by Bauer and colleagues not only provides a valuable new insight into the pathogenesis of liver derangements in sepsis, but even more importantly, establishes a model that should be welcomed and embraced by scientists working in the field."
Advertisement
Source-Eurekalert