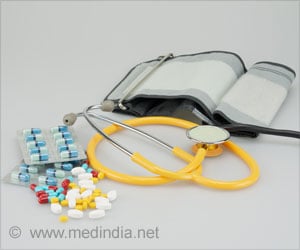
Dexmedetomidine, a drug is used after surgery and in the intensive care unit (ICU) to reduce postoperative delirium may work by preventing the overactivity of certain receptors in brain cells.

TOP INSIGHT
Dexmedetomidine, a drug is used after surgery and in the intensive care unit (ICU) to reduce postoperative delirium may work by preventing the overactivity of certain receptors in brain cells. Dexmedetomidine can have adverse effects including changes in blood pressure and heart rate. Understanding how the drug works to reduce postoperative delirium, it will help to develop new potential therapies that work similarly, but with fewer side effects.
Delirium can also occur in younger patients, particularly those treated in ICUs. Until now, it has not been known how dexmedetomidine, a drug that is normally used to sedate patients, could possibly reduce delirium after surgery.
"The vast majority of patients undergo anesthesia for surgery safely, but we now appreciate that some patients develop cognitive deficits that are unexpected and may last after anesthetics wear off," said lead researcher Beverley A. Orser, M.D., Ph.D., professor and chair of the Department of Anesthesia at the University of Toronto.
"Postoperative delirium is associated with poor long-term outcomes, including prolonged hospitalization, loss of independence and even increased mortality. There are many factors that likely contribute to cause postoperative delirium, including pre-existing medical conditions, medications, electrolyte imbalance and inflammation in the brain."
To function normally, the brain relies on a delicate balance between chemicals that excite nerve cells and chemicals that inhibit nerve cells. γ-aminobutyric acid (GABA), the major inhibitory chemical in the brain, plays a crucial role in limiting brain excitability. GABAA receptors, which are expressed on the surface of cells, are the major sensors for the inhibitory chemical GABA.
In the study, researchers examined if dexmedetomidine reduced the persistent overactivity of GABAA receptors caused by anesthetics and whether it returned activity levels of GABAA receptors back to normal following general anesthesia. They studied GABAA receptor function on brain cells of healthy, young male mice. One group of mice received only the anesthetic drug etomidate, while the other group received both the etomidate and dexmedetomidine. They studied the animals' memory and problem-solving behaviors days after the drugs had been eliminated.
"The findings may explain why this drug reduces the incidence and duration of postoperative delirium," Dr. Orser said. "While we used healthy young mice, we would expect to see the same results in older animals."
There are several reasons why it is important to understand how dexmedetomidine reduces postoperative delirium, Dr. Orser said. First, use of the drug is limited, in part because of its high cost. "Understanding how the drug reduces post-anesthetic cognitive deficits clearly strengthens the rationale for using dexmedetomidine to prevent postoperative delirium," she said.
Second, dexmedetomidine can have adverse effects including changes in blood pressure and heart rate. "If we understand how the drug works to reduce postoperative delirium, it will help us to develop new potential therapies that work in a similar way, but with fewer side effects," Dr. Orser said.
The implications of these results extend beyond the perioperative space, given that increased GABAA receptor function has been associated with several neurologic disorders including stroke, Alzheimer's disease, depression, and inflammation-induced brain injury. Dexmedetomidine, and related drugs that target a similar signaling pathway may help to prevent and treat these disorders, the authors note.
In 2016, ASA launched the Perioperative Brain Health Initiative which has engaged a multidisciplinary group to work with healthcare providers, payers and the public to create better access to care that minimizes the impact of pre-existing medical conditions that may impair intellectual abilities, and optimizes the cognitive recovery and perioperative experience for adults 65 and older undergoing surgery.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email