Surfactant replacement therapy, delivers a liquid medication for premature neonates and adults with lung injuries. The surfactant helps in lung inflation.
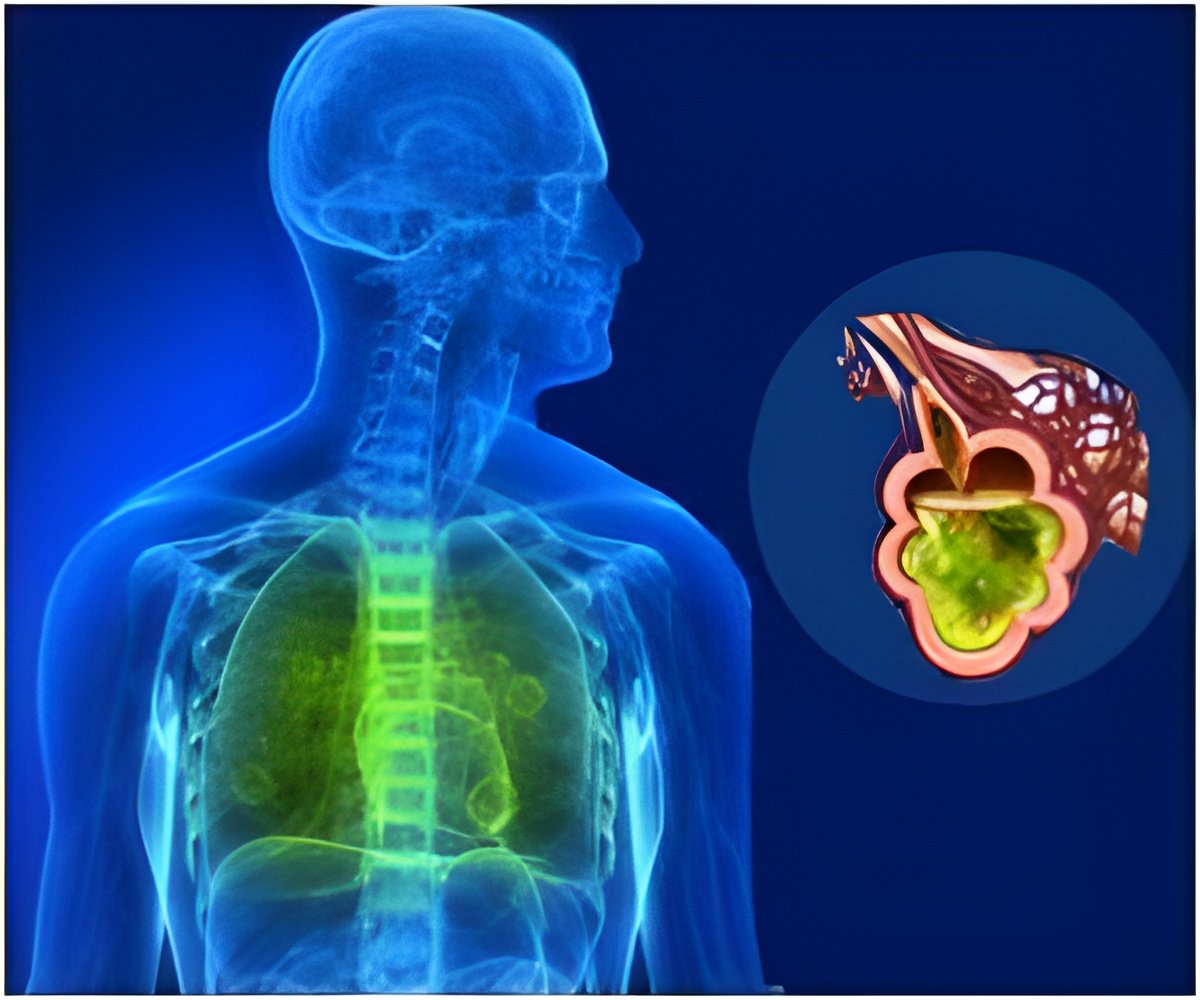
Surfactant replacement is successfully used in neonates lacking in natural surfactant, but adults with ARDS who seemingly should benefit from the therapy have shown mixed and limited results.
Surfactant replacement therapy, delivers a liquid medication into the lungs that makes it easier for them to inflate. It's widely used to treat a similar condition in premature babies, who sometimes lack the surfactant necessary to expand their lungs.
Researchers simulated the methods used in the different studies and ran them on virtual models of patient lungs to figure out which factors may be creating this disconnect. Diluted preparation of the surfactant allowed the medication to penetrate considerably deeper into the lungs reducing mortality by about half.
The same technology may be used to model patient lungs in clinical settings, extrapolating the optimal drug formulation and administration that will best fit each unique case.
 MEDINDIA
MEDINDIA

 Email
Email