A web-based lifestyle modification intervention program helps non-alcoholic fatty liver disease (NAFLD) patients to lose weight.
TOP INSIGHT
A web-based lifestyle modification intervention is much feasible in achieving weight loss in non-alcoholic fatty liver disease (NAFLD) patients.
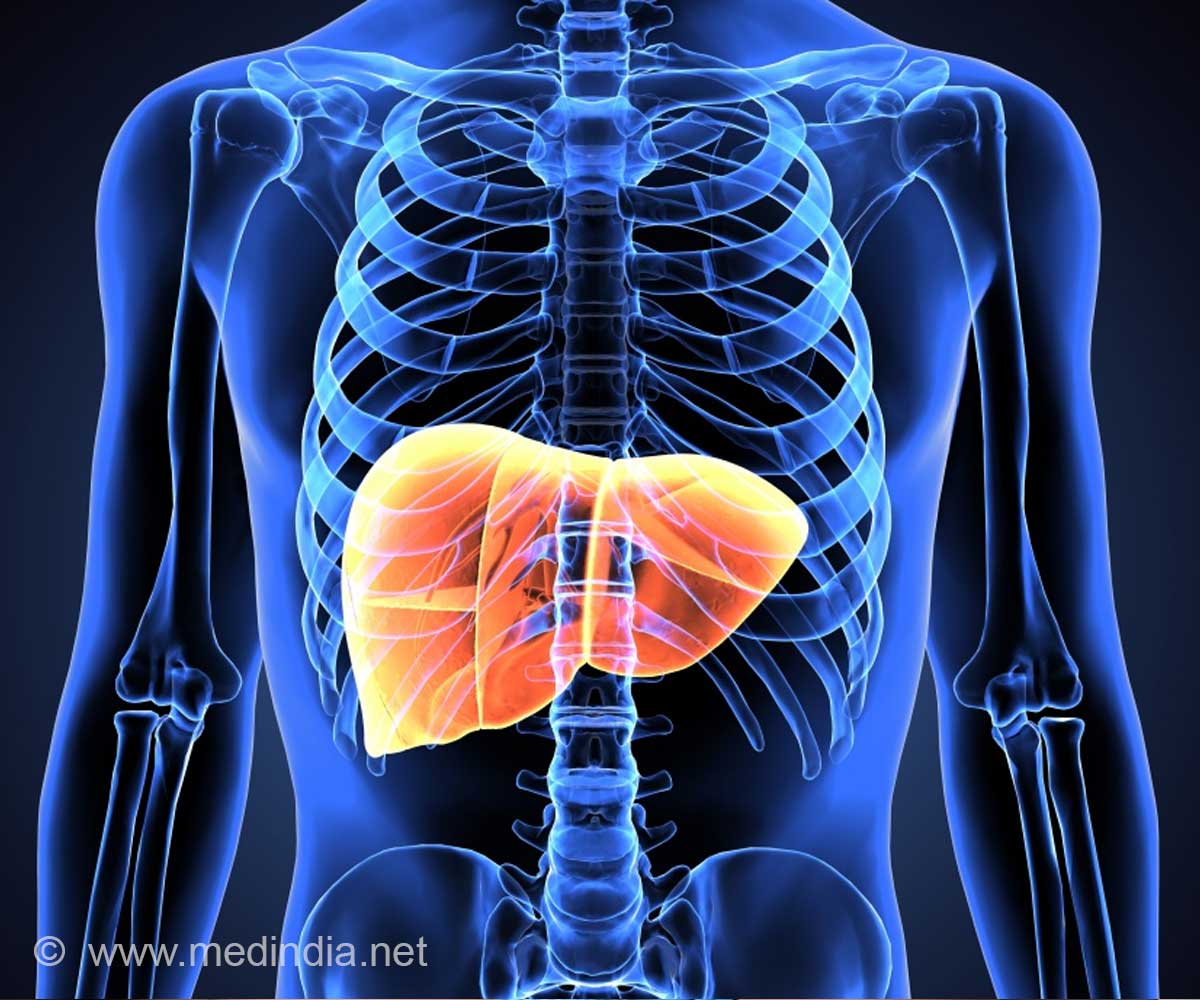
NAFLD is the most common liver disease in Western countries and is characterized by excessive hepatic fat accumulation. The global prevalence of NAFLD has been estimated to have reached 25% of adults,3 and both genetic and lifestyle factors contribute to the pathogenesis of the disease.
Lifestyle modifications geared towards weight loss, increased physical activity and improved dietary habits are central to the management of NAFLD, and structured intervention program are recommended in the guidelines.
'Lifestyle changes are mandatory for patients with NAFLD, but these are very difficult to achieve in busy clinical units', explained Prof. Marchesini.
'We wanted to develop a web-based program to help them achieve these changes, and to compare its effects with a structured, face-to-face program involving a multidisciplinary team. The participation of patients with NAFLD in structured lifestyle program may be jeopardized by job and other time constraints, and a web-based intervention may be better suited to young, busy patients'.
The web-based program included five modules, with interactive games, offline contact with the study center, and questionnaires. Surrogate markers of NAFLD severity were tested at 6-, 12-, and 24-months of follow-up. The primary outcome measure for the study was the percentage of patients who achieved 10% weight loss.
All liver enzymes decreased significantly, irrespective of the intervention, but individuals in the web-based intervention were more likely than those in the group intervention to have a normal alanine aminotransferase (ALT) level at both 6 months (OR 2.34; 95% CI 1.27, 4.30) and 12 months (OR 2.22; 95% CI 1.33, 3.73).
Surrogate markers of fibrosis decreased in both intervention groups, with statistically significant improvements from baseline observed in the Fibrosis-4 (FIB-4) index.
'Our study has shown that a web-based lifestyle modification program is a feasible and practical way of achieving a clinically meaningful level of weight loss in our NAFLD patients', said Prof. Marchesini. 'Ideally, we would now like to roll out the intervention to other liver units'.
'Weight loss has long been recognized as an effective therapy for NAFLD, but the challenge has been creating the infrastructure to achieve it', said Prof. Phil Newsome from the Queen Elizabeth Hospital and University of Birmingham, Birmingham, UK, and EASL Governing Board Member.
'Most studies have used conventional resource-intensive regimens which are not widely available in most clinical practices. This study by Prof. Marchesini demonstrates the potential of web-based approaches to achieve this at scale. The challenge now will be to see if patients are able to sustain the weight loss for longer periods of time'.
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email