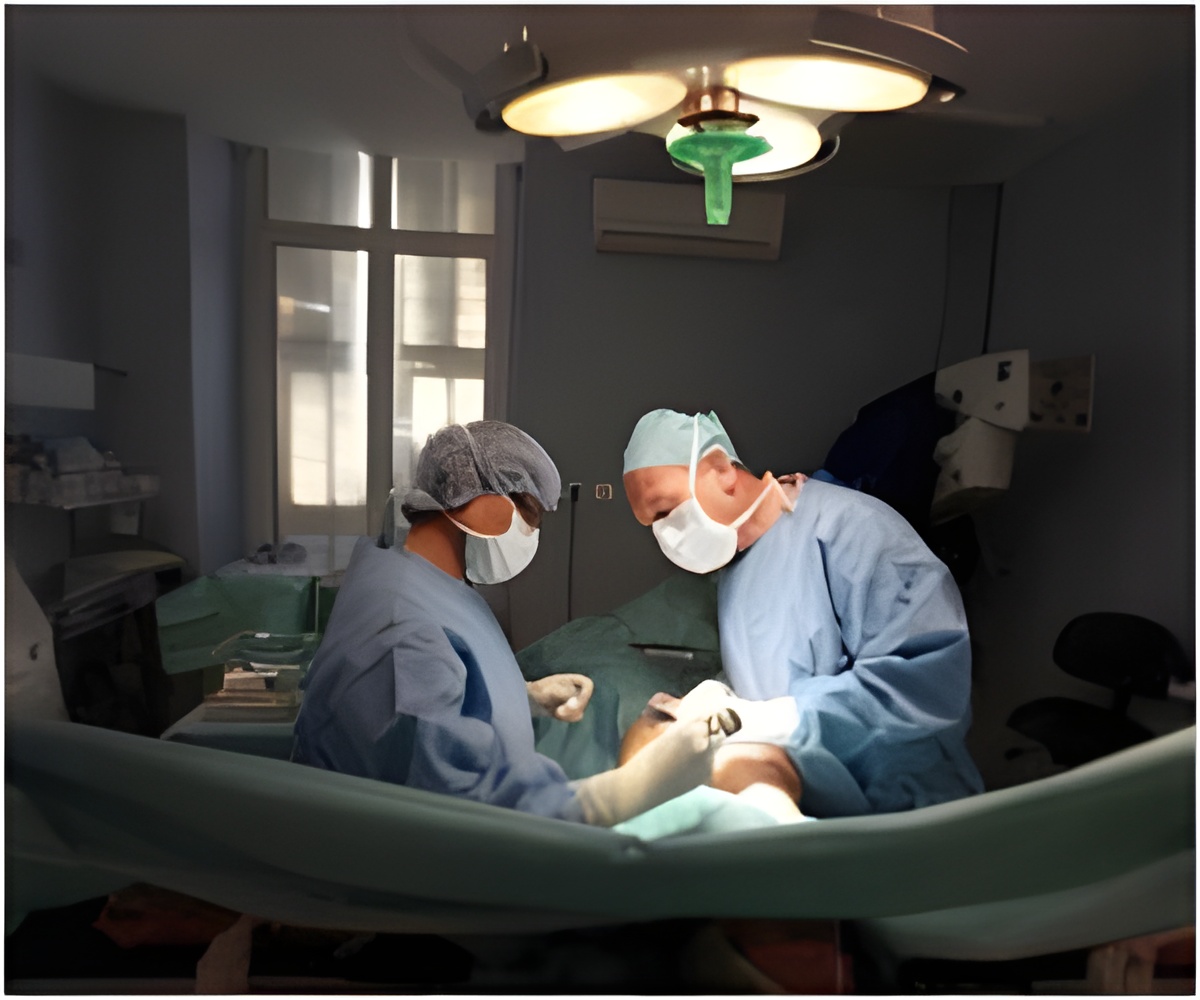
The caesarean section is a globally recognized maternal health-care indicator.
TOP INSIGHT
The richest quintile undergoing caesarean section deliveries in India has gone up from 10% to 30%, raising the country's average caesarean-section rates from 5% to 18% over the same period.
An independent analysis of data from the National Family Health Survey (1992-93 to 2015-16) and Rapid Survey on Children 2013-14 pegs India's caesarean-section rate at 18%, higher than the Lancet report's estimate of 10%.
The caesarean section is a globally recognized maternal health-care indicator: When caesarean section rates rise towards 10% across a population, maternal and newborn deaths decrease; if the rate goes above 10% - as appears to be the case in India - there is no evidence of improvement in maternal or neonatal mortality, according to a 2015 World Health Organization (WHO) statement.
State-wise data showed higher caesarean section rates in private facilities than public-health institutions. For instance, the caesarean section rate in private facilities of Tripura is close to 74% while in public institutions it is about 18%. It is the same in West Bengal, where caesarean-section rates in private and public health-care institutions are 70.9% and 18.8%, respectively.
Rajasthan has the lowest caesarean-section rates in private facilities at 23.2%, whereas Bihar has the lowest rate in public institutions at 2.6%. Telangana reported the highest caesarean-section rate in both private and public institution at 75% and 40.6%, respectively.
Telangana registers the highest incidence of C-section use in India at 58%. Caesarean section rates rose across states over a decade to 2015-16. In Tamil Nadu, percentage of caesarean-section births rose from 20.3% in 2005-06 to 34.1% in 2015-16. Goa followed at 31.4%, up from 25.7% in 2005-06.
Low-income countries reported lower rates of caesarean section (up to 10%) as compared to the middle-income and high-income countries, reported the Lancet. Worldwide, the highest caesarean-section rates are in middle-income countries, ranging between 40% and 60%.
"The reason for such high rates is less regulation in some of these countries, which are just emerging from being low-income countries, and there is an allure in technology," said Suellen Miller, one of the lead authors of the Series, and professor at the Department of Obstetrics, Gynecology and Reproductive Health, University of California, San Francisco.
Unnecessary caesarean sections also pull resources away from other services in overloaded and weak health systems.
To describe the disparity in caesarean section rates between countries and within countries, the Series' authors have coined a phrase: "Too little, too late and too much, too soon."
Too little, too late describes care with inadequate resources, and is responsible for high maternal mortality in low-income countries where women die due to lack of timely health care. Nearly five women die every hour in India from complications during childbirth with heavy blood loss caused by haemorrhage being a major factor.
Too much, too soon is a problem of high-income countries, where women experience routine over-medicalization of normal pregnancy and birth. These include induction of labor, augmentation with oxytocin (hormone), caesarean section, episiotomy (surgical cut made at opening of the vagina during childbirth), excess fetal monitoring, etc.
In 2010, over 3.5 million to 5.7 million unnecessary caesarean sections were done in high-income and middle-income countries, whereas one million to 3.5 million caesarean sections were needed but not performed in low-income countries, points out The Lancet Series.
Natural birth is a waiting game whereas the caesarean section is quick and saves time for both the doctor and the patient. Rich families can afford caesarean sections, which offer doctors better money than a vaginal delivery. Also, doctors fear repercussions (physical abuse or legal) in case something goes wrong.
"Corporate hospitals have surgical targets for doctors, which if they fail to meet, they are shown the door," said Fatima Poonawala, gynecologist and obstetrician based in Bengaluru, who was forced to quit her corporate practice. She now runs her own Afia Clinic. The figure of 10-15% caesarean section rate in India is an underestimation, she said.
"The data of National Family Health Survey and the Lancet Series is just a tip of the iceberg," said Arun Gadre, gynecologist and obstetrician, and coordinator of Pune-based NGO Support for Advocacy and Training to Health Initiatives (SATHI), which runs a campaign on health for all. Both urban and rural areas in India are facing "an epidemic of unregulated caesarean section births."
On the face of it, an overall 10% caesarean section rate in India seems acceptable. But, in reality, we need to disaggregate everything into public, private, urban, rural, wealthy, poor. The disparities are "huge and worrisome", said Miller.
Source-IANS
 MEDINDIA
MEDINDIA

 Email
Email