Phosphatidylserine (PS) biomarker for pancreatic cancer has been identified by scientists.
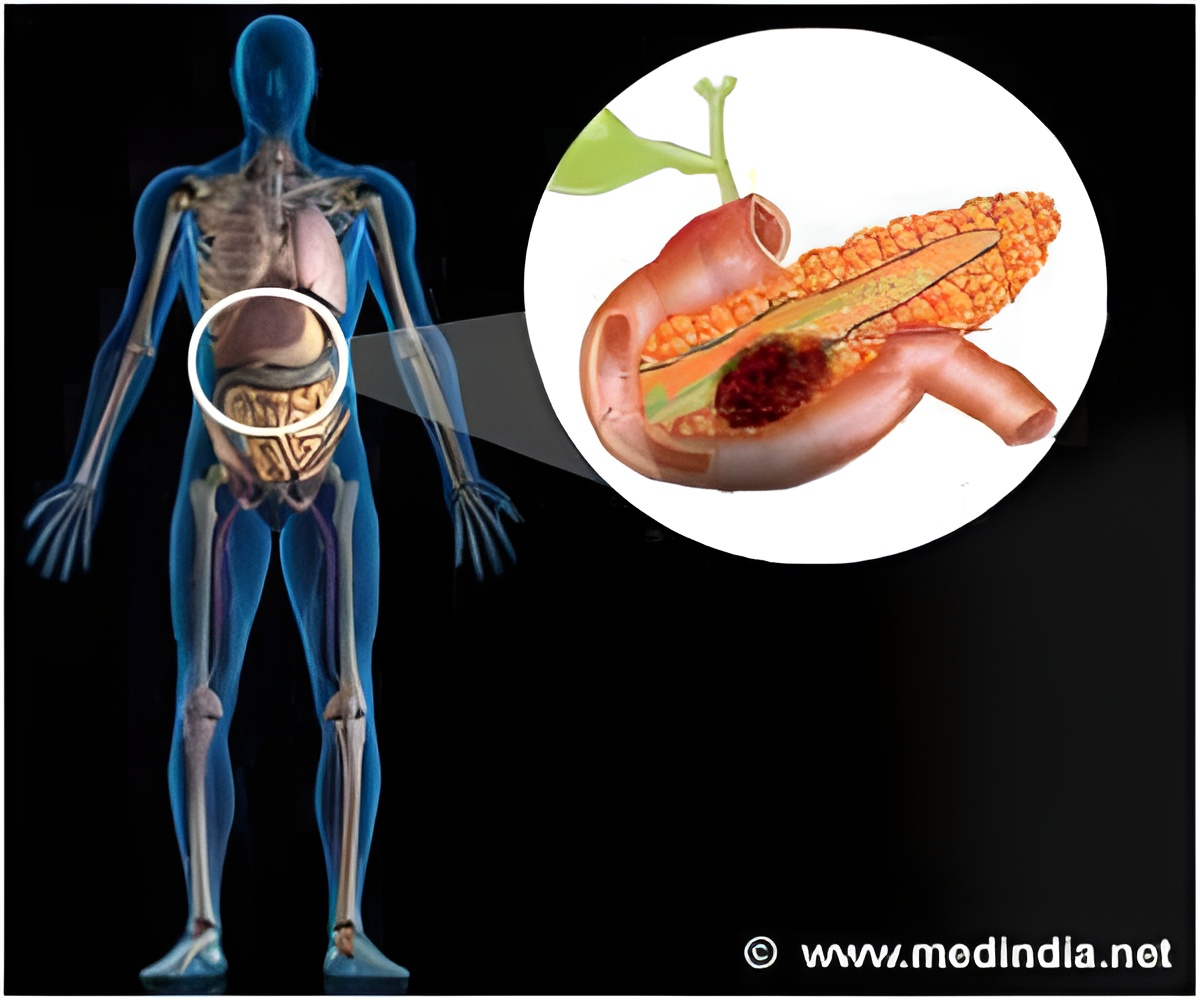
Lysosomes are membrane-enclosed organelles that contain enzymes capable of breaking down all types of biological components; phospholipids are a major components of all cell membranes and form lipid bilayers—or cell membranes.
"Only a small number of promising drugs target pancreatic cancer, which is the fourth-leading cause of cancer deaths, with a five-year survival of less than 5 percent," says Xiaoyang Qi, PhD, associate professor of hematology oncology at UC and lead researcher on the study.
"Pancreatic cancer is usually asymptomatic in the early stages, while frequently invading lymph nodes and the liver, and less often the lungs and visceral organs. Current treatments, including surgery, chemotherapy and radiation therapy, have failed to improve long-term survival."
Qi says his lab and collaborators previously found that the combination of two natural cellular components, called SapC-DOPS, which were assembled and delivered using cancer-selective nanovesicles, caused cell death in other cancer cell types, including brain, lung, skin, prostate, blood and breast cancer, while sparing normal cells and tissues.
"We also investigated the efficacy and systemic biodistribution of SapC-DOPS nanovesicles in animal models and found that it targeted and halted growth of certain cancer cells and showed no toxic effects in non-tumor tissues. In this study, we selectively targeted the cell membrane of pancreatic tumors to see if we could destroy malignant pancreatic cells without harming normal tissues and cells."
"To evaluate the role of external cell PS, we used PS exposure in human tumor and non-tumor cells via culture," he says. "We also introduced these cells into animal models and then injected the SapC-DOPS vesicles to see if changes were observed. "
To track tumor cells, human pancreatic tumor cells were illuminated with dye as well, and the same imaging device was used to identify and monitor them.
"We observed that the nanovesicles selectively killed human pancreatic cancer cells, and the noncancerous, or untransformed cells, remained unaffected," he says. "This toxic effect correlated to the surface exposure level of PS on the tumor cells."
Qi adds that animals treated with SapC-DOPS showed clear survival benefits and their tumors shrank or disappeared.
"Furthermore, using a double-tracking method in live models, we showed that the nanovesicles were specifically targeted to the tumors," he says. "These data suggest that the acidic phospholipid PS is a biomarker for pancreatic cancer that can be effectively targeted for therapy using cancer-selective SapC-DOPS nanovesicles."
"This study provides convincing evidence in support of developing a new therapeutic approach to pancreatic cancer. This technology is now being licensed and will hopefully be available in clinical trials soon."
"Dr. Qi 's discovery has great potential to be developed into diagnostics and therapies for pancreatic cancer," says Shuk-mei Ho, PhD, director of the Cincinnati Cancer Center and Jacob G. Schmidlapp Professor and Chair of Environmental Health. "This type of research helps fulfill the mission of the National Cancer Institute to promote translation of research from the bench to the bedside."
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email