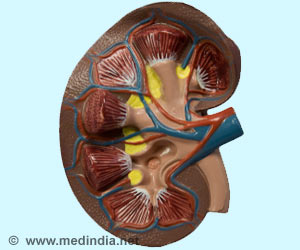
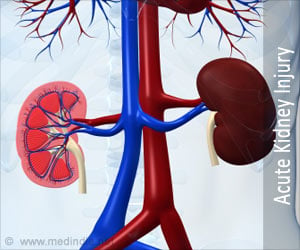
Acute renal failure develops rapidly over a few hours or days. It may be fatal. It's most common in those who are critically ill and already hospitalised.
‘AKI causes a build-up of waste products in your blood and makes it hard for your kidneys to keep the right balance of fluid in your body. AKI can also affect other organs such as the brain, heart, and lungs.’





When patients are hospitalized, they may develop AKI for a variety of reasons, with significant negative clinical consequences. To assess the healthcare costs of AKI (by degrees of severity), a team led by Scott Klarenbach, MD, MSc and David Collister, MD (University of Alberta, in Canada) studied information on adults hospitalized in Alberta between November 2002 and March 2009. Of 239,906 hospitalized patients, 25,495 (11%), 4598 (2%), 2493 (1%) and 670 (0.3%) developed AKI stages 1,2, 3 without dialysis, and 3 with dialysis, respectively. The mildest forms of AKI resulted in adjusted costs that were 1.2 to 1.3 times greater than those for patients without AKI. More severe AKI was associated with costs that were 1.8 to 2.5 times greater. Even patients who recovered from AKI had greater costs over the year after their recovery compared with patients who did not develop AKI. The incremental cost of AKI in Canada was estimated to be more than $200 million (Canadian dollars) per year.
While the incremental cost per patient was much greater for those with more severe AKI, the less severe forms of AKI resulted in greater overall costs from a population perspective. Over the time frame of admission to the hospital through a recovery period of 90 days after AKI-assessment, patients with stage 1 AKI had incremental costs of approximately CAN $3800 per patient, while patients requiring dialysis had costs of CAN $18,300; however, there were many more patients which stage 1 than stage 3 AKI. As such, the impact on healthcare resource utilization is far greater for the large number of patients with less severe forms of AKI.
"There is ongoing interest and research into strategies that prevent or reduce the severity of kidney injury, and knowledge of the healthcare costs of kidney injury is useful for both healthcare planning as well as to determine a cost-effective level of investment on preventative strategies," said Dr. Klarenbach.
Source-Eurekalert