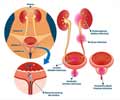
A new study from Washington University School of Medicine in St. Louis indicates that the pH level or acidity of urine and the presence of small molecules related to diet may affect susceptibility to Urinary Tract Infections (UTIs).
The research published in The Journal of Biological Chemistry may have implications for treating Urinary Tract Infections (UTIs).According to a recent analysis, a strain of bacteria called Escherichia coli or E. coli is responsible for more than 85% of all UTIs. Medicos have long relied on antibiotics to wipe out these microbes.
However, increasing bacterial resistance to these drugs has caught scientists' attention and also forced them to work on alternative treatment methods for UTIs.
As part of the mission, Dr. Jeffrey P. Henderson an assistant professor of Medicine at the University and his research team analyzed how the body normally fights bacterial infections.
The team along with first author Robin R. Shields-Cutler, cultured E. coli in urine samples from healthy people and examined main differences in how individual urine samples use the natural power of siderocalin - a key immune protein, to limit bacterial growth. Past studies have demonstrated that siderocalin helps the body to fight infections by depriving bacteria an important mineral necessary for its growth, namely iron.
The researchers divided the urine samples into two groups based on whether they restricted or permitted bacterial growth. They found that the urine samples that prevented bacterial growth supported more activity of siderocalin.
Researchers found that samples which were less acidic and closer to the neutral pH of pure water, showed a higher activity of siderocalin and were comparatively more effective at reducing bacterial growth than the acidic samples.
Most importantly, the scientists showed that they could encourage or discourage bacterial growth in urine simply by adjusting the pH level.
The scientists also linked bacterial growth to a person’s diet. They examined thousands of compounds in the urine samples to identify the presence of small metabolites called aromatics in samples that restricted bacterial growth.
Samples that almost prevented bacterial growth had more aromatic compounds compared to samples that allowed bacterial growth.
The research team says that at least some of these aromatics are excellent iron binders, helping deprive the bacteria of iron. The team further commented that these molecules are not produced by human cells but by an individual's gut microbes as they process food in the diet.
"Our study suggests that the body's immune system harnesses dietary plant compounds to prevent bacterial growth. We identified a list of compounds of interest, and many of these are associated with specific dietary components and with gut microbes," said Henderson.
The study results implicate cranberries among other possible dietary interventions.
"It's possible that cranberries may be more effective when paired with treatment to make the urine less acidic. And even then, maybe cranberries only work in people who have the right gut microbes," Henderson noted.
The investigators also showed that enterobactin is good at binding iron in urine. Therefore finding strategies to block it may help develop antimicrobial drugs that work very differently from traditional antibiotics.
References:
http://news.wustl.edu/news/Pages/A-persons-diet-acidity-of-urine-may-affect-susceptibility-to-UTIs.aspx
https://en.wikipedia.org/wiki/Urinary_tract_infection
http://www.jbc.org/
Source-Medindia