- About Toxic Shock Syndrome - (https://familydoctor.org/condition/toxic-shock-syndrome/)
- Overview - Toxic shock syndrome - (http://www.mayoclinic.org/diseases-conditions/toxic-shock-syndrome/home/ovc-20317877)
- Toxic shock syndrome (TSS) - including symptoms, treatment and prevention - (https://www.ncbi.nlm.nih.gov/pmc/articles/pmc358064)
- Toxic shock syndrome - (https://medlineplus.gov/ency/article/000653.htm)
- Toxic shock syndrome (TSS) - (https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/toxic-shock-syndrome-tss)
- What is Toxic Shock Syndrome? - (http://www.sahealth.sa.gov.au/wps/wcm/connect/public+content/sa+health+internet/health+topics/health+conditions+prevention+and+treatment/infectious+diseases/toxic+shock+syndrome/toxic+shock+syndrome+tss+-+including+symptoms+treatment+and+prevention)
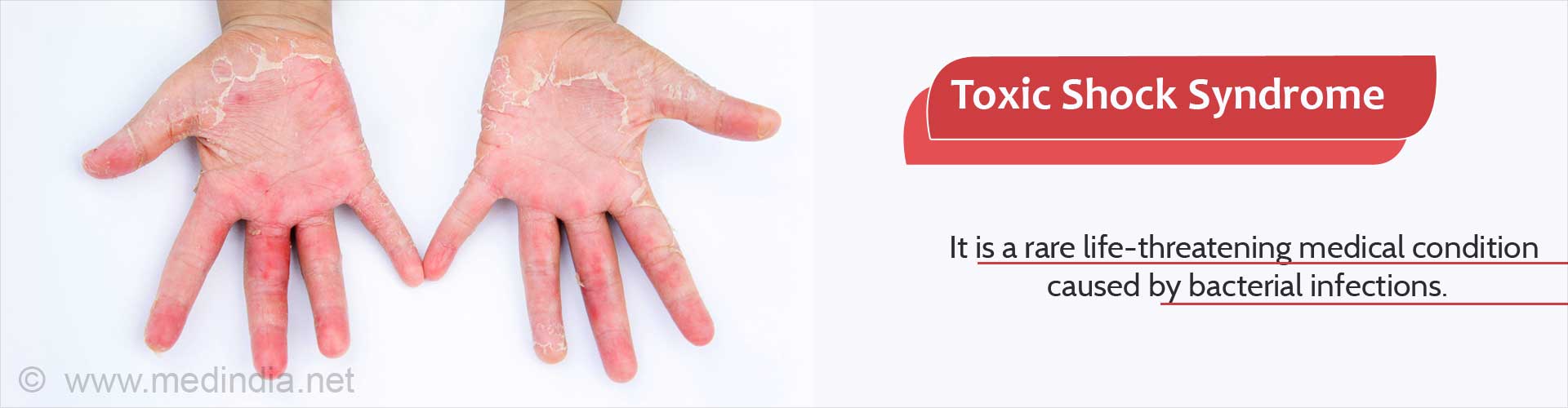
What is Toxic Shock Syndrome?
Toxic shock syndrome is a rare life-threatening medical condition caused by bacterial infections. Most commonly, the disease is linked to the use of superabsorbent tampons during menstruation. However, it can affect both men and women of all ages, including children. The incidence rate of toxic shock syndrome (TSS) caused by Staphylococci is more than 50% in menstruating women; the remaining of them occur in older women, men and children. TSS caused by Streptococci affects people of all ages.
What are the Causes of Toxic Shock Syndrome?
Bacterial infections lead to toxic shock syndrome. The toxins produced by bacteria Staphylococcus aureus and Streptococcus pyogens enter the bloodstream and produce symptoms of toxic shock syndrome. Once the bacteria find a favorable environment, they grow rapidly and release toxins into the bloodstream. The following are the main reasons for the production of bacterial toxins:
- Use of tampons during menstruation. When a tampon is left for duration of more than 4-8 hours in the vagina, it creates a favorable environment for the bacteria to grow due to the presence of the shed blood.
- Use of birth control devices such as diaphragms and contraceptive sponges for a longer duration than recommended.
- Infectious deep wounds, delay in wound healing after surgery or burn can encourage bacterial growth.
- Skin infections.
- The dressing used to stop nose bleeding is a potential risk factor.
- It can occur soon after childbirth in the birth canal of the mother.
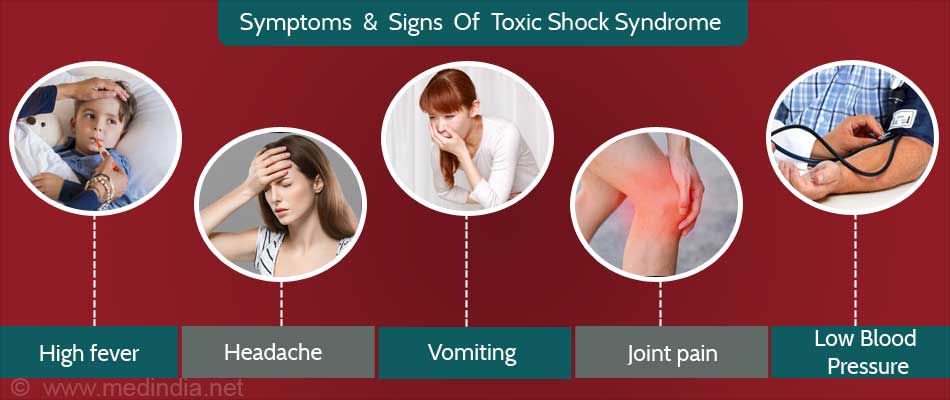
What are the Signs and Symptoms of Toxic Shock Syndrome?
Signs and symptoms of toxic shock syndrome vary according to the type of infection and the bacteria causing it. Nonetheless, the most common ones are as follows:
- High fever
- Headache
- Vomiting
- Low blood pressure (Hypotension)
- Sore throat
- Joint pain
- Sensitivity to light
- Mental confusion and disorientation
- Diarrhea
- Muscle pain (Myalgia)
- Fatigue
- Low platelet count
- Redness of eyes, mouth, nose, throat, and vagina
- Seizures
- Necrosis (soft tissue destruction)
- Presence of sunburn-like red rashes and peeling patches on the palms and bottom of the feet may begin within 2-3 weeks after the infection.
- At an advanced stage, toxic shock syndrome may lead to multiple organ failure chiefly involving the kidneys and liver.
How do you Diagnose Toxic Shock Syndrome?
There is no accurate diagnostic test for toxic shock syndrome. However, a number of tests are run to confirm the diagnosis.
- Clinical confirmation of symptoms such as high fever, fall in blood pressure, peeling of the skin from the palms and feet by physical examination of the patient.
- Blood tests are done to check the presence of bacterial infection. A complete blood count shows a low platelet count in case of toxic shock syndrome. Three might also be high white blood cell count, high neutrophil count as well as high ESR (erythrocyte sedimention rate) that indicate an infection.
- Urine test is performed to check for the presence of bacterial infection related to Staphylococcus aureus and Streptococcus pyogenes.
- Swab test is performed to detect the presence of infection in the vagina, cervix, and throat.
- In an advanced stage of toxic shock syndrome, vital organs may get affected. Imaging tests like CT scan and chest X-ray are conducted to assess the extent of damage to the organs.
How do you Treat Toxic Shock Syndrome?
The treatment for this condition depends on the patient and the extent of illness.
- The first line of treatment is immediate admission to a tertiary care hospital.
- Oxygen support for breathing.
- Antibiotics are administered intravenously to kill the infection-causing bacteria.

- Fluids are injected intravenously to treat dehydration.
- To maintain normal blood pressure, medicines are prescribed.
- Infected contraceptive devices, if present, are removed.
- The infected wound, if any, will be cleaned thoroughly.
- Kidney dialysis is preformed if required.
- Surgery is recommended to remove dead tissue from the site of infection, if any.
How do you Prevent Toxic Shock Syndrome?
Toxic shock syndrome can be prevented by taking the following precautions -
- Changing tampons frequently.
- Limit the use of tampons and use sanitary pads instead.
- Get wound dressing changed on regular basis, every day ideally.
- Check for any symptoms associated with toxic shock syndrome and consult a doctor as soon you notice them.
- Maintain optimal personal hygiene.

What is the Prognosis of Toxic Shock Syndrome?
Toxic shock syndrome can prove to be fatal if left untreated. With early diagnosis and proper treatment, patients can recover within 2-3 weeks. However, almost 50% cases have been recorded to be fatal.
Health Tips
Use light absorbent tampons or sanitary napkins and wash hands before and after insertion of tampons. Change tampons frequently every 4-8 hours.
Change the dressing of wound to keep it clean.