Q: Which doctor should I consult for neuropathy?
A: A General Practitioner (GP) would clinically evaluate and may recommend a withdrawal or change in the medication known to cause neuropathy. Based on the observed therapeutic response or continued adverse effect of the drug, the GP may then refer to a specialist, a neurologist or a neuromuscular neurologist who can advise further on the medicines.
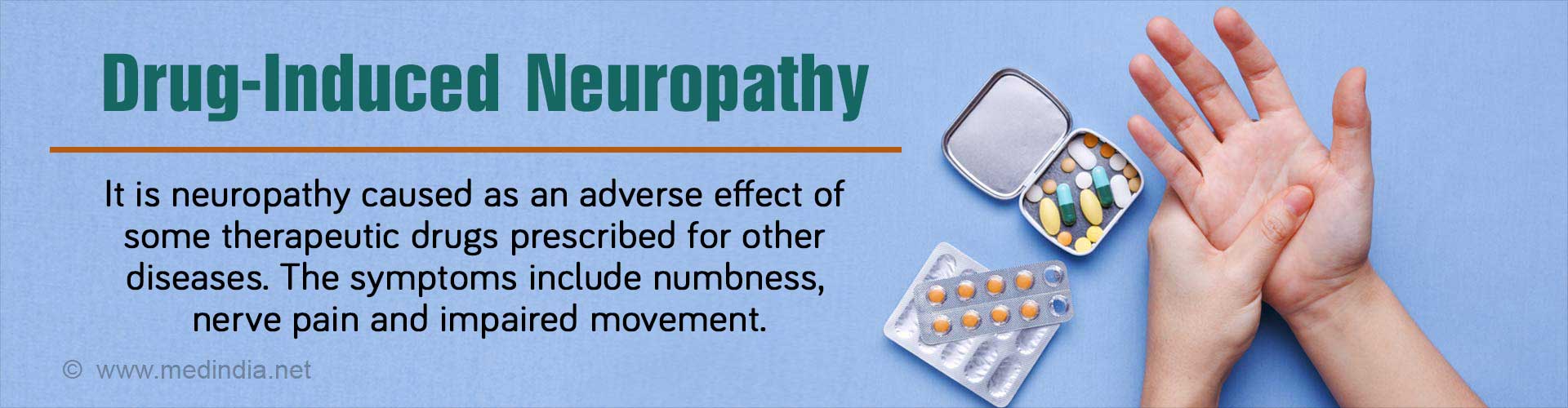
Q: Who gets drug-induced neuropathy?
A: Patients who are on drugs which are known to cause neuropathy as an adverse effect get drug-induced neuropathy. It can affect anyone, regardless of age and gender.
Q: What are the medicines and substances which may lead to the development of neuropathy?
A: Some medicines like chemotherapy drugs, for example, cisplatin, anti-cholesterol drugs like statins, and exposure to toxic substances like lead, mercury, and arsenic may lead to the development of neuropathy.
Q: What areas are affected by peripheral neuropathy?
A: All areas except brain and central nervous system get affected by peripheral neuropathy. These areas include the heart, digestive system, vascular system, urinary system, and the system controlling sweat and tears.
Q: Are peripheral neuropathy and Multiple Sclerosis the same?
A: No, they are different. Peripheral neuropathy affects the peripheral nerves and transmission of right signals back to the brain. In Multiple sclerosis, the damage is to the brain, wherein the brain fails to transmit the correct signals to the peripheral nerves.
Q: Do all neuropathies cause pain?
A: No, all neuropathies do not cause pain; some may only interfere with movement and control of muscles.
Q: What vitamins are good for neuropathy condition?
A: A diet or supplements that are rich in Vitamin B6 and Vitamin B12 help in reducing pain due to diabetic neuropathy.
 MEDINDIA
MEDINDIA
 Email
Email