Neuroscientists using functional magnetic resonance imaging have come closer to learning how differently wired psychopaths are that they don't feel empathy and concern when others are in pain.
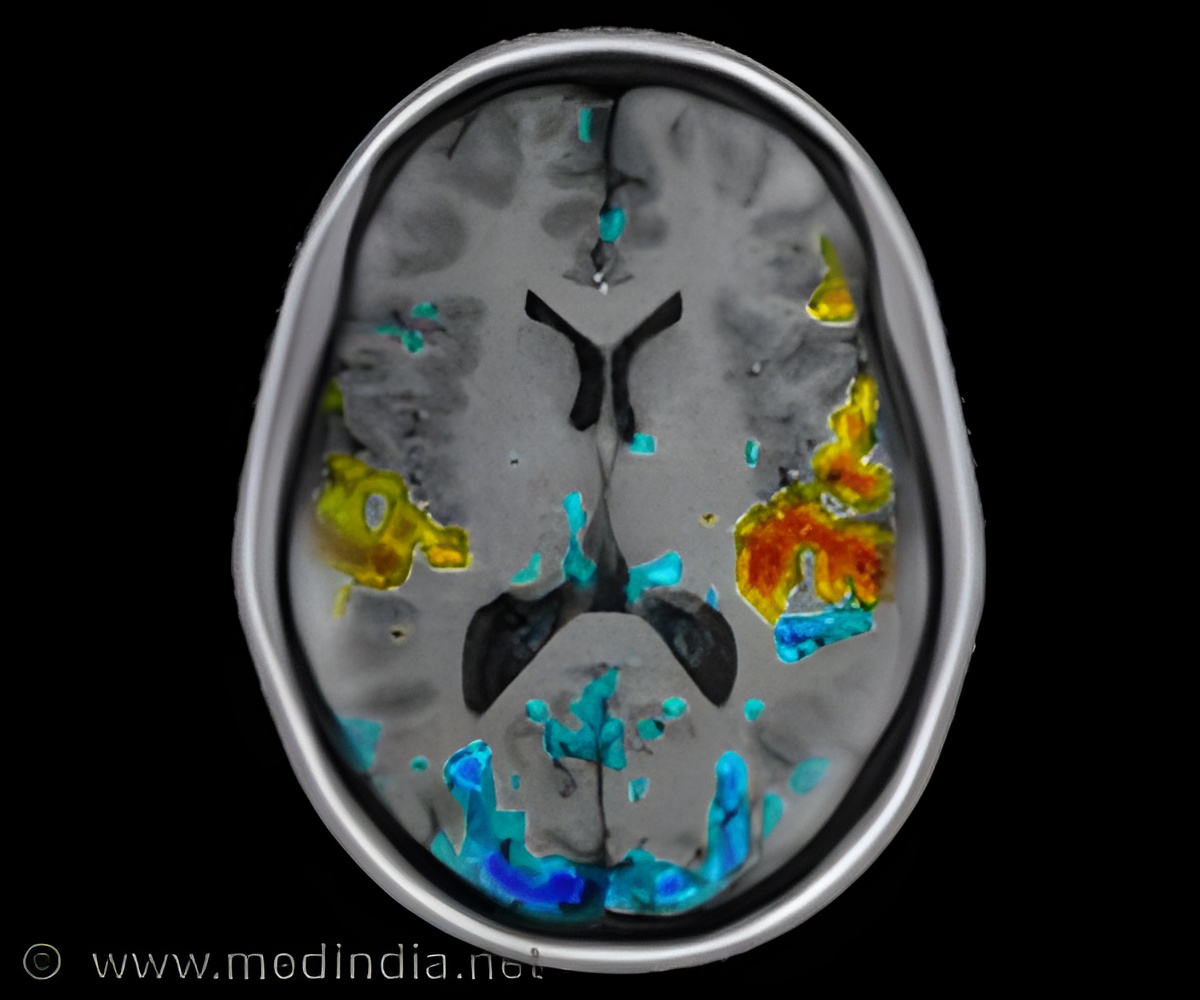
To better understand the neurological basis of empathy dysfunction in psychopaths, neuroscientists used functional magnetic resonance imaging (fMRI) on the brains of 121 inmates of a medium-security prison in the USA.
Participants were shown visual scenarios illustrating physical pain, such as a finger caught between a door, or a toe caught under a heavy object. They were by turns invited to imagine that this accident happened to themselves, or somebody else. They were also shown control images that did not depict any painful situation, for example a hand on a doorknob.
Participants were assessed with the widely used PCL-R, a diagnostic tool to identify their degree of psychopathic tendencies. Based on this assessment, the participants were then divided in three groups of approximately 40 individuals each: highly, moderately, and weakly psychopathic.
When highly psychopathic participants imagined pain to themselves, they showed a typical neural response within the brain regions involved in empathy for pain, including the anterior insula, the anterior midcingulate cortex, somatosensory cortex, and the right amygdala. The increase in brain activity in these regions was unusually pronounced, suggesting that psychopathic people are sensitive to the thought of pain.
But when participants imagined pain to others, these regions failed to become active in high psychopaths. Moreover, psychopaths showed an increased response in the ventral striatum, an area known to be involved in pleasure, when imagining others in pain.
Taken together, this atypical pattern of activation and effective connectivity associated with perspective taking manipulations may inform intervention programs in a domain where therapeutic pessimism is more the rule than the exception. Altered connectivity may constitute novel targets for intervention. Imagining oneself in pain or in distress may trigger a stronger affective reaction than imagining what another person would feel, and this could be used with some psychopaths in cognitive-behavior therapies as a kick-starting technique, write the authors.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email




