Risk Of Soft Tissue Sarcomas In Hereditary Retinoblastoma Survivors - A Study Finds
A study by Ruth A. Kleinerman and his colleagues quantifies the risk of hereditary retinoblastoma survivors developing specific subtypes of soft tissue sarcomas and finds that this risk persists for decades after the original retinoblastoma diagnosis.
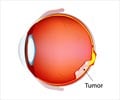
The findings published in the January 3 issue of the Journal of the National Cancer Institute emphasizes the importance of regular medical surveillance for these patients, the authors say.Retinoblastoma is a rare cancer of the retina that primarily affects children and is most often diagnosed before age 1. The disease can often be cured; 97 percent of retinoblastoma patients survive 5 years after diagnosis.
However, patients with hereditary retinoblastoma are at a high risk of developing another cancer, including soft tissue sarcomas. The increased risk of soft tissue sarcomas is attributed both to the mutation in the RB-1 gene that causes retinoblastoma and to the radiation treatment that most retinoblastoma patients received when treated decades ago. Radiation is used less frequently today because of the risk of second cancers.
The researchers at the National Cancer Institute in Bethesda, Md., studied a group of 963 1-year hereditary retinoblastoma survivors to better understand the risks for specific subtypes of soft tissue sarcomas. The patients were diagnosed between 1914 and 1984 at medical centers in New York and Boston and were followed for an average of 25.2 years. More than half of the patients were younger than 1-year-old when diagnosed, and most (88.2 percent) of the patients were treated with radiation.
A total of 69 soft tissue sarcomas were diagnosed in 68 hereditary retinoblastoma patients. The most common subtype was leiomyosarcoma, a cancer of smooth muscle cells that was diagnosed in 23 of the patients. Other frequently diagnosed sarcomas were fibrosarcoma (13 patients), malignant fibrous histiocytoma (12), rhabdomyosarcoma (8), and liposarcoma (3). The authors calculated that there was a 184-fold increase in soft-tissue sarcomas among hereditary retinoblastoma survivors compared with the general population and a 390-fold increase in cases of leiomyosarcomas.
Only 20 percent of the soft tissue sarcomas were diagnosed within 10 years of the retinoblastoma diagnosis; 45 percent of the sarcomas arose 30 or more years after diagnosis. In addition, 18 of the 23 (78 percent) leiomyosarcomas were diagnosed 30 or more years after the diagnosis of retinoblastoma. Almost all sarcomas were diagnosed in retinoblastoma survivors who had been treated with radiation. However, 18 of the 69 sarcomas developed outside the original radiation treatment field, and leiomyosarcoma was diagnosed more often outside the radiation field than in it.
"Given the excellent survival of retinoblastoma patients, it is important that survivors continue to undergo regular medical surveillance for sarcomas in their adult years," the authors write.
"The importance of this [new] report lies in its emphasis on leiomyosarcoma, a tumor that occurs in RB-1 gene carriers whether or not they were treated with radiation and that can be expected to continue to occur in older survivors, who will require more careful follow-up."
Source-Eurekalert
SRI
 MEDINDIA
MEDINDIA
 Email
Email