According to research North Carolina's coordinated, regional systems for rapid care improved survival rates of patients suffering from the most severe heart attack.
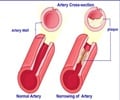
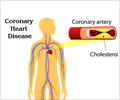
Each year, nearly 300,000 people in the United States have a STEMI, which occurs when a blood clot completely blocks an artery to the heart. Permanent damage and disability can often be prevented by rapidly restoring the blood flow.Researchers analyzed the Regional Approach to Cardiovascular Emergencies (RACE) project, which involves regional care systems supporting voluntary coordination between emergency medical services (EMS) and all hospitals with emergency departments, including competing hospitals. "The most important care decisions for heart attack patients are made long before they get to the hospital," said James G. Jollis, M.D., the study's lead author and a professor of medicine and radiology at Duke University in Durham, N.C.
"These coordinated care systems should be in every single hospital and every single EMS system in the country."Full implementation of the RACE system involved collaboration with thousands of healthcare professionals in 119 hospitals and more than 500 EMS agencies across North Carolina. Researchers reviewed records from July 2008 to December 2009, when more than 7,000 patients were treated (average age 59, 30 percent women).
The EMS technician training and hospital guidelines in RACE are based on standards established through the American Heart Association's Mission: Lifeline® STEMI program. The goal of Mission: Lifeline STEMI is to have patients receiving artery-opening treatment within 90 minutes of their initial contact with the healthcare system. That first contact includes paramedics for patients who call 911 or the hospital emergency department for patients who use their own transportation to the hospital. "The paramedics have the ability to identify the STEMI and, when needed, call to alert the catheterization team from the ambulance," Jollis said. "When they arrive, the patient is taken straight to cath lab and most ― 52 percent ― are treated within 60 minutes."
The STEMI care system also outlines when and how patients are transferred if they need treatment at a hospital that provides interventional cardiac catheterization. With RACE coordinated care systems, transferred patients got to cardiac surgery within 103 minutes of arriving at the first hospital, compared to 117 minutes prior to the system implementation. Furthermore, specialty cardiac centers in RACE accept all patients whether or not beds are available after surgery.
"Our study shows coordinated regional STEMI systems save lives, no matter what unique challenges are posed by geographical or healthcare settings," said Christopher Granger, M.D., study co-author and a cardiologist at Duke. Building on the success of the North Carolina system, RACE investigators are working with Mission: Lifeline leaders to establish additional regional STEMI systems across the country. This program, the Mission: Lifeline® STEMI Systems Accelerator demonstration project, launches this summer in 20 regions across the country."With appropriate coordination of emergency and hospital care, this system can be replicated and should be a model for the standard of care everywhere to save many more lives," Granger said.
Advertisement