People nearing the end of their lives - even those enrolled in hospice - can experience multiple transitions between places where they receive care.

TOP INSIGHT
People nearing the end of their lives - even those enrolled in hospice - can experience multiple transitions between care settings.
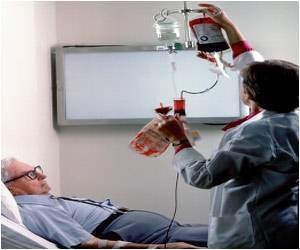
Such transitions included transferring from and to a hospital, skilled nursing facility, home health agency, hospice, or home. The researchers said that they considered these specific transitions because they were those most likely to mean changes in the patient's care team, which could lead to uncoordinated care.
Of the 311,090 people included in the study:
- 10.2% (31,675) experienced at least one healthcare transition after their hospice enrollment.
- 6.6% of hospice patients had more than one care transition, some up to 19 transitions.
- Of those transitions, more than half were to a hospital.
Those who experienced care transitions tended to be younger or non-white, had more than one chronic condition, or received in-patient hospice care compared to those who did not experience transitions.
The number of transitions varied widely from state to state, ranging from 6.9% of study subjects in Idaho to 20.6% of study subjects in Florida. The proportion of people who had a transition to a hospital ranged from 1.6% in North Dakota to 13.4% in Mississippi.
"Even after being enrolled in hospice, Medicare beneficiaries may have numerous transitions between different healthcare settings. These transitions are not only expensive, but also may not lead to better care or quality of life. Many of these transitions may be avoidable through advance care planning, appropriate provider-to-provider communication, and proper hospice inpatient care," said study co-author Shiyi Wang, Assistant Professor of Epidemiology, Yale School of Public Health.
 MEDINDIA
MEDINDIA



 Email
Email