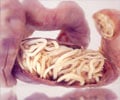
The severity of infection from Toxoplasma gondii could depend on the damage suffered by the nerve cells, according to a new Johns Hopkins study.
The findings of the new study, published in the March issue of the journal Infection and Immunity, help explain why the infection causes serious disease in some but not in others and clarify its role in psychiatric disorders, the researchers say.
The discovery could help physicians predict the severity of an infection by strain type and tailor treatments accordingly, it is hoped.
“We already know that toxoplasmosis can play a role in some psychiatric disorders, but up until now we didn’t know why. Working with human nerve cells, our study shows the exact alterations triggered by each strain that can eventually manifest themselves as symptoms,” says senior investigator Robert Yolken, M.D., a neurovirologist at Johns Hopkins Children’s Center.
The researchers injected human nerve cells with the three most common toxoplasma strains, each of which caused a different pattern of gene expression. One of the most basic functions in all living organisms, gene expression occurs when a gene is switched on to release a substance that tells cells what to do or not do, determining the cells’ biologic behavior. Gene expression can be turned on and off, stepped up or down by various factors, including viral and bacterial invasions.
Cells infected with toxoplasma type I — the most virulent strain in mice — had the greatest impact on gene expression, altering more than 1,000 genes, 28 of them linked to brain development and central nervous system function and 31 others to nerve impulse and signaling.
A handful of genes were affected by all three strains, notably a gene called VIPR2 that regulates neurotransmitters and nerve signaling and may play a role in schizophrenia, the researchers say.
A 2008 study by Yolken and colleagues revealed that toxoplasma infection increases the risk for schizophrenia and could precipitate the disease in genetically predisposed people, a classic example of how genes and environment come together in the development of disease.
Most infections with toxoplasma occur early in life following exposure to the parasite from cat feces or undercooked beef or pork. Farm animals and rodents also get infected, but the parasite reaches full sexual reproduction only in cats. Infections rarely cause symptoms, but the parasite remains in the body and can reactivate after lying dormant for years.
Co-investigators on the study included Lorraine Jones-Brando, M.D., and C. Conover Talbot Jr., both of Hopkins. The research was funded by the Stanley Medical Research Institute.
Source-Medindia
 MEDINDIA
MEDINDIA
 Email
Email