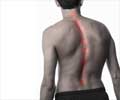
Scoliosis is an abnormal lateral curvature of the spine. It is most often diagnosed in childhood or early adolescence, but can also be diagnosed in adults.
Scoliosis is an abnormal lateral curvature of the spine. It is most often diagnosed in childhood or early adolescence, but can also be diagnosed in adults. The spine's normal curves occur at the cervical, thoracic, and lumbar regions in the so-called “sagittal” plane. These natural curves position the head over the pelvis and work as shock absorbers to distribute mechanical stress during movement.
“Scoliosis that occurs or is diagnosed in adulthood is distinctive from childhood scoliosis, since the underlying causes and goals of treatment differ in patients who have already reached skeletal maturity,” stated Roger Hartl, MD, a spine surgeon and American Association of Neurological Surgeons (AANS) spokesperson. Most adults with scoliosis can be divided into the following categories: 1) Adult scoliosis patients who were surgically treated as adolescents; 2) Adults who did not receive treatment when they were younger; and 3) Adults with a type of scoliosis called degenerative scoliosis.Degenerative scoliosis occurs most frequently in the lumbar spine (lower back) and more commonly affects people age 65 and older. It is often accompanied by spinal stenosis, or narrowing of the spinal canal, which pinches the spinal nerves and makes it difficult for them to function normally. Back pain associated with degenerative scoliosis usually begins gradually, and is linked with activity. The curvature of the spine in this form of scoliosis is often relatively minor, so surgery may only be advised when conservative methods fail to alleviate pain associated with the condition.
There are several signs that may indicate the possibility of scoliosis. If you notice one or more of the following signs, the AANS recommends that you schedule an appointment with a doctor.
· Shoulders are uneven – one or both shoulder blades may stick out
· Head is not centered directly above the pelvis
· One or both hips are raised or unusually high
· Rib cages are at different heights
· Waist is uneven
· The appearance or texture of the skin overlying the spine changes (dimples, hairy patches, color abnormalities)
· The entire body leans to one side.
If the doctor suspects scoliosis after performing a physical examination, radiological tests will be ordered to confirm diagnosis. In adults with scoliosis, x-rays are usually recommended once every five years, unless symptoms are getting progressively worse.
In one 20-year study, about 40 percent of adult scoliosis patients experienced a progression. Of those, 10 percent showed a very significant progression, while the other 30 percent experienced a very mild progression, usually of less than one degree per year. Progression of a curve depends on factors such as age of diagnosis, age and efficacy/outcome of original treatment, and both severity and location of the curvature.
“Bracing is not an option for adults as a primary treatment because their spines have reached maturity and are no longer growing,” said Dr. Hartl. However, bracing may be used postoperatively in adults to keep the spine straight while it heals.
A number of factors can lead to increased surgical-related risks in older adults with scoliosis. These factors include: advanced age, being a smoker, being overweight, and the presence of other health/medical problems. In general, both surgery and recovery time are expected to be longer in older adults. The benefits of spine surgery should always be weighed against its risks.
Source-Newswise
SRM/J
 MEDINDIA
MEDINDIA
 Email
Email