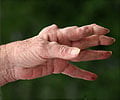
New research published today in Nature Medicine says that a signal molecule made by the human body that triggers the immune system into action may be important in rheumatoid arthritis.
New research published today in Nature Medicine says that a signal molecule made by the human body that triggers the immune system into action may be important in rheumatoid arthritis.
The authors of the study, from Imperial College London, say that if scientists could block this signal, it may be possible to develop more effective arthritis treatments.Rheumatoid arthritis is the most common autoimmune disease, affecting around 1 in 100 people. It causes painful and persistent swelling in the joints that can result in damage to the bone and cartilage. Around half of all patients do not respond to one or more of the treatments currently available, and even these can become less successful over time. The researchers behind the new study say stopping the disease closer to the root of the problem could be the best way to treat it, and their results suggest a new target for therapies.
When a microbe infects the body, the body responds by turning on a molecular switch to set the immune system into action and protect the body from disease. Today's findings show that a signal molecule called tenascin-C can trigger the same molecular switch and also activate the immune system. High levels of tenascin-C present in joints therefore may cause the activated immune system to attack the joint leading to the persistent inflammation of rheumatoid arthritis.
The molecular switch is called TLR4, and is found on the surface of immune cells. Previous research has shown that mice without TLR4 do not show chronic joint inflammation. The researchers hope scientists can develop new treatments that target the interaction between tenascin-C and TLR4, which may help to combat rheumatoid arthritis.
Dr Kim Midwood, lead author of the study from the Kennedy Institute of Rheumatology at Imperial College London, said: "Rheumatoid arthritis is a debilitating and painful disease and, unfortunately, there is no cure. Furthermore, current treatments are not effective for many patients."
"We have uncovered one way that the immune system may be triggered to attack the joints in patients with rheumatoid arthritis. We hope our new findings can be used to develop new therapies that interfere with tenascin-C activation of the immune system and that these will reduce the painful inflammation that is a hallmark of this condition," added Dr Midwood.
In a subsequent study, the researchers injected the active part of the tenascin-C molecule into mice joints. They found it caused the joints of the mice to become inflamed and that this reaction was more intense with higher doses.
The authors plan to work out the precise mechanism by which tenascin-C increases these levels of inflammatory molecules in the human joint and try to find ways to inhibit this action.
Source-Eurekalert
RAS
 MEDINDIA
MEDINDIA


 Email
Email