The largest study ever of its kind, with more than 10,000 patients from 20 countries, has revealed that removing blood clot as a treatment for heart attacks is not beneficial.
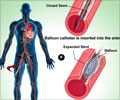
It showed there was no benefit from the routine use of thrombectomy, or blood clot removal, and that heart attack patients receiving this were more likely to have a stroke compared to those undergoing percutaneous coronary intervention (PCI) alone. PCI, also known as angioplasty, is a common procedure that involves opening up a blocked artery in the heart usually with a balloon followed by a stent.
"The message from this study is that thrombectomy should not be used as a routine strategy," said lead author Dr.Sanjit Jolly, an associate professor of medicine of McMaster’s Michael G. DeGroote School of Medicine. "This is still an important therapy, but given the downsides we observed in our trial, its use should be quite selective and as a measure when an initial balloon angioplasty attempt fails to open up the artery, rather than as a routine strategy."
In manual thrombectomy, the cardiologist uses a syringe attached to a tube to create suction to remove the clot from the artery.
Jolly, who is also an interventional cardiologist with HHS, said earlier studies suggested this treatment may be beneficial and said that "it makes sense that if you prevent the blood clot from going downstream and blocking little branches that you could potentially reduce the size of the heart attack and improve outcomes; however we did not observe that in our trial".
Current guidelines leave it to physicians to decide whether to routinely perform thrombectomy during PCI or use it only as a backup strategy in cases where the angioplasty fails to open the blockage.
After six months of follow-up, the study revealed no differences between patients who received PCI alone versus those who also received manual thrombectomy, in terms of a combination of the rates of cardiovascular death, subsequent heart attack, cardiogenic shock and the most severe category of heart failure.
The researchers saw no difference in outcomes based on the size of the blood clots, despite previous speculation that the procedure might be particularly beneficial in patients with larger clots.
"There are still open questions that aren’t resolved by our study," said Jolly. "Clearly, for patients who fail an initial angioplasty attempt, thrombectomy is really the only way to open up the artery."
Dr. Vlad, the study’s co-principal investigator who is a professor of medicine at the University of Toronto and an interventional cardiologist at the Peter Munk Cardiac Centre, University Health Network, said: "We did not design the trial to test the effectiveness of selective or bailout thrombectomy," adding, "Thrombectomy remains an important treatment when the patient’s blood vessel is still filled with blood clot when the PCI procedure is done, or if it cannot be completed successfully because of the clot."
Previous smaller studies have suggested benefits of routine thrombectomy or showed mixed results, but these studies involved fewer patients and some were limited to a single hospital.
"Our findings illustrate the importance of doing large trials," said Jolly. "There are many things in clinical practice that we believe are beneficial but need to be tested in large randomized trials. Only by doing this can we be certain of what helps patients and move the field forward."
Source-Newswise
 MEDINDIA
MEDINDIA



 Email
Email