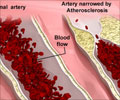
Patients with genotype 1 chronic hepatitis C virus (HCV) infection have a high risk of suffering from early atherosclerosis
In the first study, researchers led by Dr. Salvatore Petta from the Di.Bi.M.I.S. University of Palermo in Italy evaluated 174 patients with chronic HCV (genotype 1) along with 174 controls from an outpatient cardiology unit for signs of atherosclerosis. Ultrasonography was used to measure thickening of the carotid artery. Severity of fibrosis was determined for all HCV patients.
The team found carotid plaques in 42% of HCV patients compared to 23% of patients in the control group. Older age and severe liver fibrosis were independently associated with the presence of carotid plaque according to the authors. In patients 55 years or younger who had less sever fibrosis (stage F0-F2) only 22% had plaques in their artery compared to 52% with more sever fibrosis (stage F3-F4). Patients older the 55 years of age had similar prevalence of carotid lesions for those with or without severe fibrosis at 58% and 51% respectively.
"Our findings suggest that severe liver fibrosis places chronic HCV patients at higher risk of early atherosclerosis," said Dr. Petta. "This patient group should be carefully monitored to prevent progression of cardiovascular disease that is independent of their metabolic profile." The authors also caution that a majority of the European study participants were overweight, which should be considered in applying results to other patient populations.
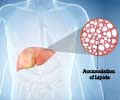
A second study by Dr. Michaela Kozakova and colleagues from the University of Pisa further explored whether the association between fatty liver disease and early atherosclerosis is a consequence of shared conventional risk factors or is it determined by a specific circulating factor originating from liver or adipose tissue. For this purpose the researches investigated the association between the presence of early carotid plaques and the fatty liver index (FLI), which is an established surrogate marker for fatty liver disease based on body mass index (BMI), waist circumference, triglycerides and gamma glutamyltransferase (GGT), in subjects who were part of the multicenter European RISC (Relationship between Insulin Sensitivity and Cardiovascular risk) study group. For the present study, a subgroup of 1.012 RISC subjects who were free of hypertension, diabetes, cardiovascular diseases, chronic hepatic, inflammatory and neoplastic diseases, abnormal lipid levels, and metabolic syndrome were included.
In such a healthy population, only about 5% of subjects had small carotid plaques, and these subjects were older, had a FLI of 60 or more, and had higher blood pressure, LDL cholesterol, glucose, GGT and C-reactive protein than participants without plaques. In logistic regression model, after adjustment for conventional cardiovascular risk factors, family history, liver transaminase and alcohol consumption, the independent predictors of plaque presence were age, FLI of 60 or more and smoking habit. However, when FLI in the model was replaced by variables used in its equation the predictors of early atherosclerosis were age, GGT and smoking.
 MEDINDIA
MEDINDIA

 Email
Email