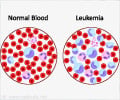
A new, pre-clinical study by researchers suggests that a novel drug combination could lead to profound leukemia cell death by disrupting the function of two major pro-survival proteins.

In the study, published in the journal Cancer Research, researchers combined the drug ABT-737 with another agent BEZ235. ABT-737 targets proteins known as B-cell lymphoma 2 (Bcl-2) and Bcl-xL, which prevent apoptosis, a form of cell suicide, in cancer cells. BEZ235 directly inhibits the PI3K/AKT/mTOR pathway, and as a result, reduces the expression of another anti-apoptotic protein known as Mcl-1, which is not targeted by ABT-737.
Among their many functions, signaling pathways regulate biological processes required for cellular survival. The PI3K/AKT/mTOR pathway helps keep apoptosis in check, in part, by controlling the production of Mcl-1. However, the pathway can become dysregulated in cancer, and in so doing, contribute to uncontrolled tumor growth and resistance to conventional cancer therapies.
It is activated in 50 to 80 percent of patients with acute myelogenous leukemia (AML), and in some, but not all cases, is associated with genetic mutations. Significantly, disabling both anti-apoptotic proteins, Bcl-2 and Bcl-xL, in conjunction with Mcl-1, caused profound cell death of leukemia cells in the test tube as well as in animal models of AML.
"This study builds on many years of work in our laboratory investigating the mechanisms that regulate apoptosis in human leukemia cells. To the best of our knowledge, it is the first to raise the possibility that activation of the P13K/AKT/mTOR pathway, rather than genetic mutations within the pathway, may represent the best predictor of leukemia cell responses to these targeted agents," says one of the study's key researchers Steven Grant, M.D., Shirley Carter Olsson and Sture Gordon Olsson Chair in Oncology Research, associate director for translational research, program co-leader of Developmental Therapeutics and Cancer Cell Signaling research member at VCU Massey Cancer Center.
"These findings could lead to a new therapeutic strategy for patients with AML and potentially other diseases by targeting patients whose leukemia cells display activation of a specific survival pathway."
Advertisement
Moving forward, Grant and his team hope to work with pharmaceutical companies and the National Cancer Institute to develop strategies combining inhibitors of the PI3K/AKT/mTOR pathway with Bcl-2 family antagonists for the treatment of patients with AML.
Advertisement