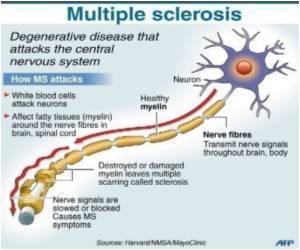
New research on the relationship between multiple sclerosis (MS) and chronic cerebral venous insufficiency (CCSVI) may be a result of MS, not a cause.
Robert Zivadinov, MD, PhD, associate professor of neurology in the UB School of Medicine and Biomedical Sciences and president of the International Society for Neurovascular Disease, is first author on the paper.
Zivadinov says of the findings: "Given the intense interest in the hypothesis that CCSVI is a possible cause of MS, independent evaluation of CCSVI was identified as an urgent need.
"Our results indicate that only 56.1 percent of MS patients and 38.1 percent of patients with a condition known as clinically isolated syndrome (CIS), an individual''s first neurological episode, had CCSVI.
"While this may suggest an association between the MS and CCSVI, association does not imply causality. In fact, 42.3 percent of participants classified as having other neurological diseases (OND), as well as 22.7 percent of healthy controls involved in the study, also presented with CCSVI.
"These findings indicate that CCSVI does not have a primary role in causing MS," says Zivadinov. "Our findings are consistent with increased prevalence of CCSVI in MS, but substantially lower than the sensitivity and specificity rates in MS reported originally by the Italian investigators."
Advertisement
Zamboni''s original investigation in a group of 65 patients and 235 controls showed that CCSVI appeared to be strongly associated with MS, increasing the risk of having MS by 43 fold.
Advertisement
The study group consisted of 289 persons with MS, 163 healthy controls, 26 with OND and 21 with CIS.
MS patients also were defined by disease type: relapsing-remitting (RR), secondary progressive (SP), primary-progressive (PP), progressive-relapsing (PR) and MS with neuromyelitis optical (NMO) -- a type of MS that affects the optic nerves and spinal cord exclusively.
All patients underwent transcranial and extracranial echo-Doppler scans of the head and neck. Persons were considered "CCSVI-positive" if they met two or more of five venous hemodynamic (VH) criteria.
Prevalence rates were calculated in three groupings: only subjects with positive and negative CCSVI diagnoses; only borderline cases included in the negative group; and subjects who fulfilled any of the five criteria.
When only positive and negative CCSVI cases were considered, results showed a CCSVI prevalence of 62.5 percent in MS patients, 45.8 percent in those with OND, 42.1 percent in CIS, and 25.5 percent in healthy controls.
When borderline cases were included as negative for CCSVI, prevalence figures were 56.1 percent in MS patients, 42.3 percent in those with OND, 38.1 percent with CIS and 22.7 percent in healthy controls.
When all cases that met at least one of the five VH criteria were included in the analysis, CCSVI prevalence was 81.3 percent in MS cases, 76.2 percent in CIS patients, 65.4 percent in OND cases and 55.2 percent in healthy controls.
The highest prevalence was seen in relapsing primary-progressive MS (89.4 percent), followed by non-relapsing secondary-progressive MS (67.2 percent), NMO (66.6 percent), primary-progressive MS (54.5 percent) and relapsing-remitting MS (49.2 percent). CCSVI prevalence was substantially higher in progressive MS than in non-progressive MS patients. In addition, patients with a progressive MS disease subtype had higher CCSVI prevalence than those with non-progressive MS.
"The higher prevalence of CCSVI in progressive MS patients suggests that CCSVI may be a consequence, rather than a cause, of MS," says Bianca Weinstock-Guttman, MD, co-principal investigator of the study and UB professor of neurology. Therefore, the possibility that CCSVI may be a consequence of MS progression cannot be excluded and should be further investigated.
"Several studies have reported that patients with progressive MS show decreased blood flow through the brain''s neuronal tissue, indicating that CCSVI may be secondary to reduced perfusion," says Weinstock-Guttman. "In addition, we recently showed an association between the severity of CCSVI and reduced cerebral blood flow in brain parenchyma of MS patients in an published pilot study."
E. Ann Yeh, MD, UB assistant professor of neurology and a major collaborator on the study, noted that of the 10 pediatric MS patients who participated in the study, five presented with CCSVI (50 percent), yielding prevalence similar to that in adult MS patients.
"Although the sample size was too small to draw any firm conclusions, these results suggest that CCSVI is also present in children and is not the result of aging," she says.
Concludes Zivadinov: "The differences between our study, the original Italian CCSVI study and other recently published studies also emphasize the need for a multimodal approach for the assessment of CCSVI. In addition to Doppler sonography, use of selective venography, magnetic resonance venography and intraluminal Doppler methods can provide more evidence for the true prevalence of CCSVI in MS."
Additional UB researchers involved in this research are: Karen Marr, Murali Ramananthan, PhD, Ralph H. B. Benedict, PhD, Cheryl Kennedy, MPH, Makki Elfadil, MD, Justine Reuther, Christina Brooks, Kristin Hunt, Michelle Andrews, Ellen Carl, Michael G. Dwyer and David Hojnacki, MD. Gary Cutter, PhD, from the Department of Biostatistics, University at Alabama, Birmingham, also played a critical role in the research.
The study was supported by the Buffalo Neuroimaging Analysis Center, Baird MS Center and the Jacobs Neurological Institute, all from UB, as well as the Direct MS Foundation, the Jacquemin Family Foundation and more than 500 individual donors.
The University at Buffalo is a premier research-intensive public university, a flagship institution in the State University of New York system and its largest and most comprehensive campus. UB''s more than 28,000 students pursue their academic interests through more than 300 undergraduate, graduate and professional degree programs. Founded in 1846, the University at Buffalo is a member of the Association of American Universities.
Source-Newswise