While human embryonic stem cells hold great promise for studying and treating disease and for the practice of regenerative medicine, more must be learned to ensure their safety
Chromosomal and genetic variations found in human embryonic stem cells lines have been attributed, in large part, to the various culture conditions in which they're grown, said Tamar Dvash, first author of the study and a postdoctoral fellow at UCLA.
However, the work by the Broad Stem Cell Research Center scientists reveals that very early in their growth, female human embryonic stem cells already show variation in the inactivation of the X chromosome.
"It suggests that culture conditions and methods in the derivation of human embryonic stem cells could be further improved to achieve a uniform pattern of X chromosome inactivation," said Guoping Fan, an associate professor of human genetics and senior author of the study.
The study is published June 25, 2010 in the early online edition of the journal PLoS ONE, a publication of the Public Library of Science.
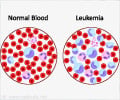
All female cells have two X chromosomes and in early development, one X chromosome is permanently inactivated. The X chromosome inactivation ensures that females, like males, have one functional copy of the X chromosome in each body cell and that the cells develop normally. If the second X chromosome is not inactivated, the result could be disease development, including some cancers in which two active X chromosomes can be found in the malignant cells, Dvash said.
Advertisement
The creation of a stem cell line includes many steps. The donated, frozen blastocysts are thawed and the inner cell mass – the 20 to 50 cells that are fully pluripotent in the blastocyst - is placed in culture with cells that support its growth. After a time, a small piece of the developing stem cell colony, or group of cells, is cut away and placed into a culture dish to further expand, a process called passaging.
Advertisement
"People are looking at these cells as having great potential for transplantation and possible cures for diseases," Dvash said. "What this study proves is that we need to monitor X chromosome inactivation closely in cells being considered for therapeutic use. We need to make sure they're undergoing normal inactivation to ensure they will be stable when they begin to differentiate."
Going forward, the scientists will also examine induced pluripotent stem cells, adult stem cells that have been reprogrammed to have all the qualities of embryonic stem cells, which can become any cell in the body. They will study skin cells taken from females, which would already have undergone inactivation of one X chromosome because they are already differentiated. The cells will be programmed into embryonic-like cells with two active X chromosomes so they can more closely study the process of inactivation.
"We want to know how does it happen and when," Dvash said.
Source-Eurekalert