A significantly lower risk of stroke, heart and renal disease is linked to the use of a new technique that removes the nerves connecting the kidney to the brain
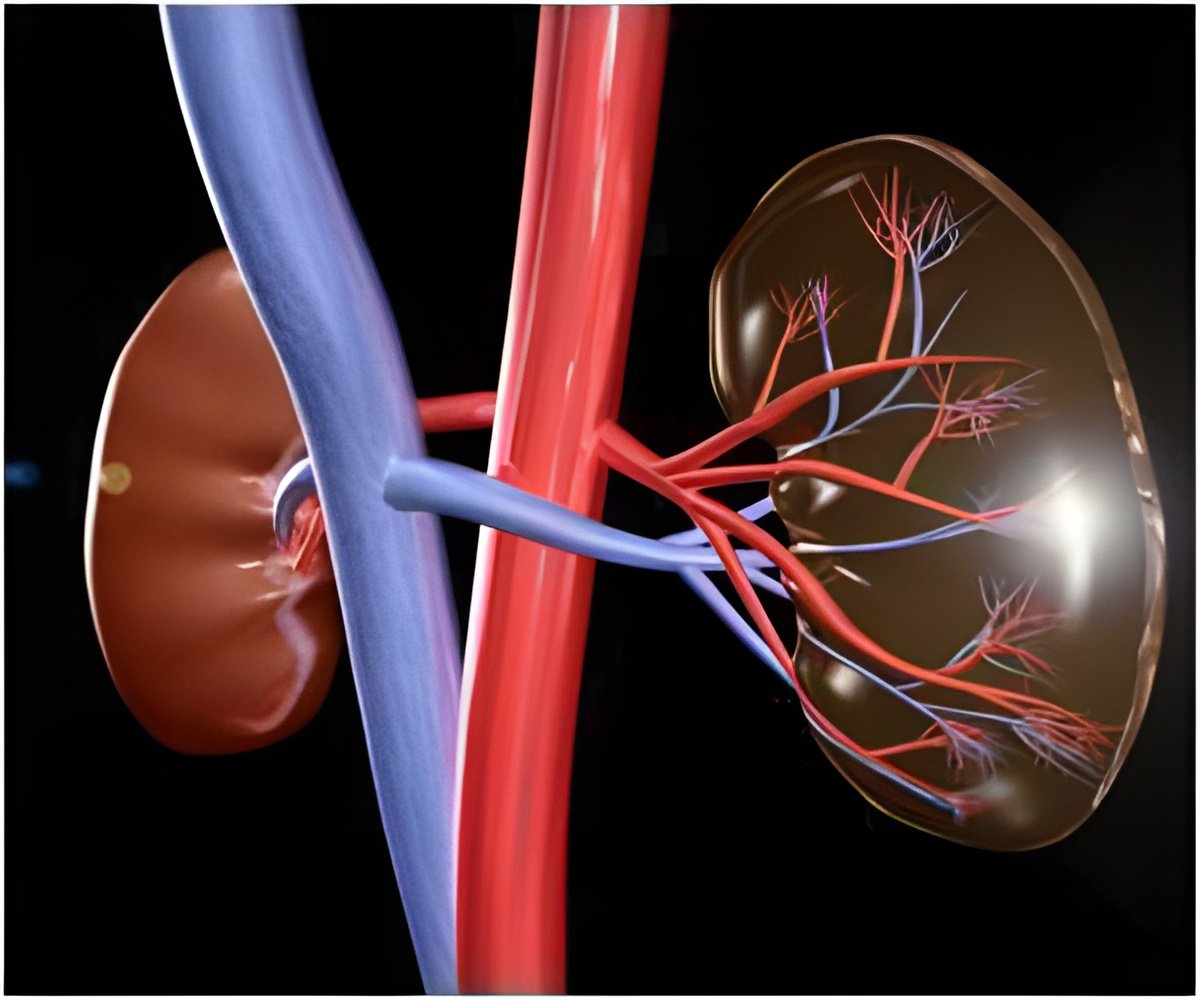
Inspired by these results, cardiologists Dr Angus Nightingale and Dr Andreas Baumbach from the Bristol Heart Institute (BHI) adopted the technique called "renal denervation" to remove the nerves to the kidney in patients with high blood pressure.
The procedure, which has been successfully trialled on 19 patients at the BHI, is performed using a fine tube that is inserted in an artery in the patient's leg and positioned in the artery feeding blood to the patient's kidneys. The nerves to the kidney are around the artery and ablated by radio-frequency energy that is emitted from the tube.
The breakthrough is due to a new collaboration involving scientists at the University of Bristol and cardiologists at the BHI, who have joined forces to form the CardioNomics high blood pressure team. Together, they hope to tackle this major health problem by taking findings from the laboratory and translating them into clinical practice. The CardioNomics team have just been awarded £100,000 grant from Medtronic to further improve the technique and expand patient trials.
Dr Nightingale, who runs the Specialist Hypertension Clinic at the BHI, said: "We have used renal denervation in patients who have hard-to-treat blood pressure. Similar to the results from the basic science experiments, we have also seen reductions in blood pressure which has been essential for reducing the risk of heart and renal disease, and stroke in our patients. This is an exciting new treatment for these patients who have struggled with high blood pressure which tablets are not controlling."
Dr Baumbach, an interventional cardiologist who performed the treatment, added: "The technique is very straight forward, performed as a day case and there are no side-effects. It is becoming a popular technique for patients with both resistance and poor tolerability to high blood pressure medication."
 MEDINDIA
MEDINDIA


 Email
Email