Even after years of research on the bacterium responsible for causing tuberculosis, scientists did not have an explanation of how it managed to adapt to changing conditions in the host.
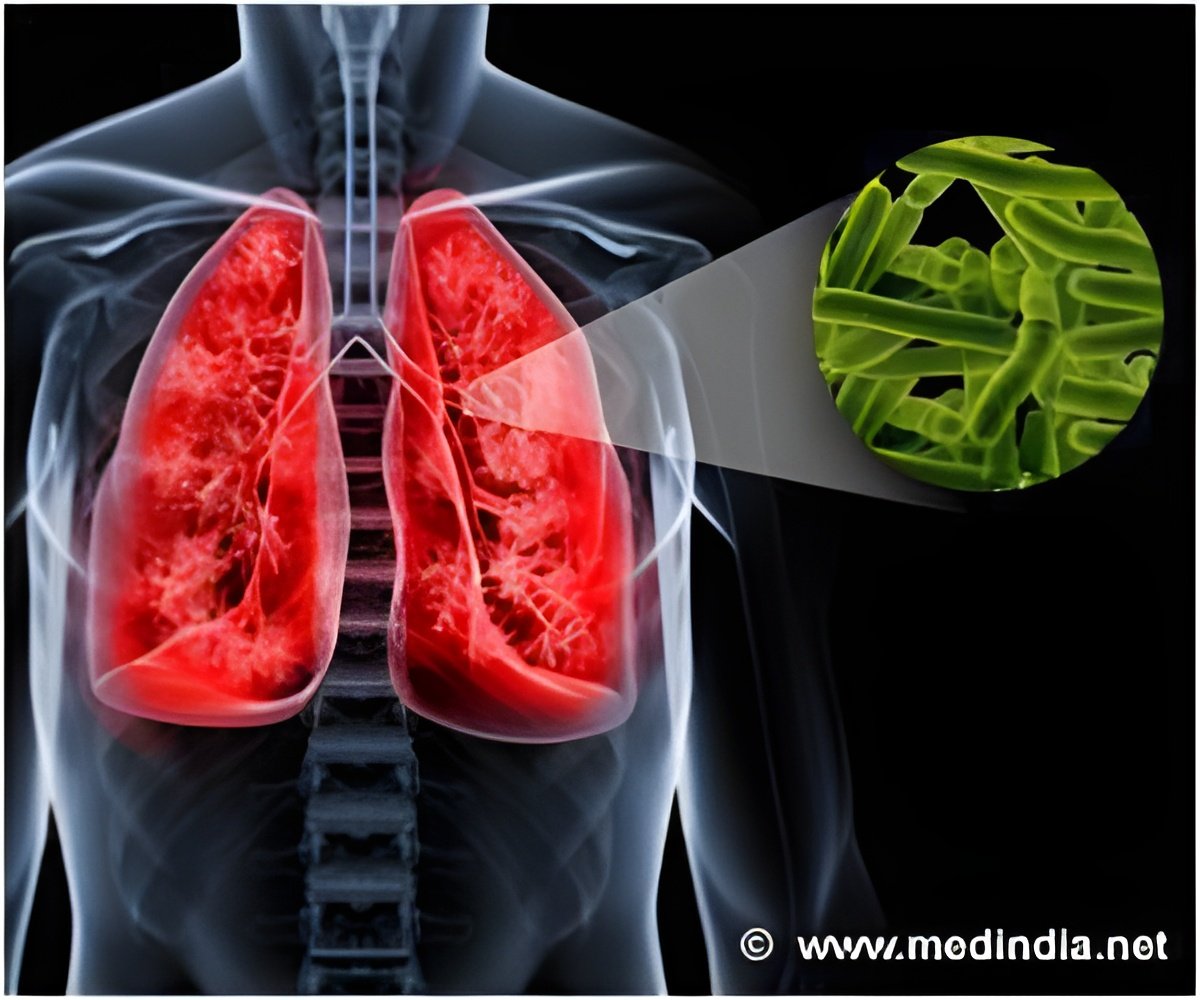
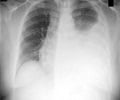
One third of the world's population is latently infected with TB, harboring the bacteria in a dormant form in the lungs. In 2011 alone, 8.7 million people fell ill with the active form of TB, and 1.4 million died.
For hundreds of years, people have associated reduced oxygen tension with the control of TB. Artificially collapsing an infected lung using a pneumothorax device, or inserting golf ball-sized items into the pleural cavity, were common ways to treat the disease before the rise of antibiotics. Despite the prevalence of these treatment methods, the bacteria appeared to survive in the host, even in hypoxic environments.
"We needed a window into how tuberculosis adapts to change, whether that is a lack of oxygen or a new drug," explains David Sherman, Ph.D., a lead researcher from Seattle BioMed. "In order to do that, we needed to understand how TB is wired—how its genes and the molecules that regulate them are related—so we can see how it changes its behavior depending on the environment."
Mapping tuberculosis
In order to create a map of how TB genes are regulated, researchers led by Gary K. Schoolnik, Ph.D., at the Stanford Medical School, David Sherman, Ph.D., of Seattle BioMed and James E. Galagan, Ph.D., of Boston University and the Broad Institute, turned to technologies that identified the key players in the system. Using ChIP-Seq, a method to analyze how proteins interact with DNA, they identified where 50 of TB's regulatory transcription factors bound to DNA, thereby providing the wiring diagram of genetic connections.
Creating a road map for future interventions
"Everyone who studies TB can now look at this wiring diagram and gain a better understanding of how their favorite genes relate in a larger context," he says. "Suddenly, we can see how different areas connect, in intimate and important detail."
Though this map is the most comprehensive to date, Sherman and his colleagues plan to fill it out even further by incorporating the sequences of the remaining transcription factors and their relationship to the TB genome. The map will eventually provide a window into how targeted drugs or immunological interventions could interfere with TB's ability to survive in the host, adding a critical weapon to the fight against TB's worldwide devastation.
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email