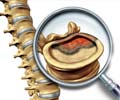
People paralyzed by spinal cord injuries have been offered a new hope after Otago University researchers claimed the wounds could soon be repaired using cells from patients' noses.
Otago University researchers recommend the use of “nose’s cells” for treating spinal cord injuries and hence, avoiding possible paralysis.
The New Zealand's Health Ministry's ethics committee has approved an application by the Spinal Cord Society, which will open the way for a clinical trial involving 12 patients.Noela Vallis, the society's president, said there was no shortage of volunteers ready to take part.
"Some have already gone overseas out of a sense of frustration that they can't access it ie the experimental treatment here," the NZPA quoted Vallis, as saying.
Research director Jim Faed, who heads the Spinal Cord Society's lab at Otago University, and his team is focusing on two promising cell types: one is a kind of adult stem cell produced by a patient's own bone marrow.
However, researchers are likely to begin trials using olfactory ie scent receptor cells from the patient's nose, injecting them into damaged spinal cord.
"The olfactory tissue in the nose is unique because it is the only place in the body where there is constant replacement of nerve cells throughout life," Dr Faed said.
The nasal tissue acts like "nurse cells", providing growth factor hormone to nerve cells, enabling them to make "meaningful connections".
The Otago group is in contact with Portuguese neuropathologist Carlos Lima, who pioneered that trial.
Faed said some participants experienced side effects, but they were "few and manageable" and none had been fatal. Positive benefits for patients included return of some muscle function and sensation in parts of the body, which previously had no feeling, he said.
Faed said the Dunedin lab hoped to get full approval for the trial before Christmas, and would then begin recruiting patients. The first 12 could start treatment next year.
Source-ANI
TAN
 MEDINDIA
MEDINDIA


 Email
Email