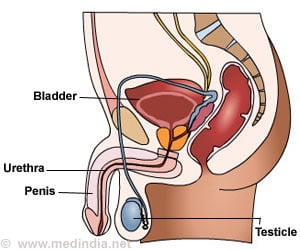
Proper development of the fetal penis requires not just testosterone from the testes, but a second hormone produced by other tissues, including the placenta.
‘Penis development was shown to also depend on a second process, called the alternative or "backdoor" pathway, which also ends in the production of DHT but doesn't depend on the production of testosterone by the testes.’





To learn more about this pathway, the authors used mass-spectrometry to measure levels of different steroids in fetal plasma and tissue during the second trimester, when the most critical steps in penis development occur. They also analyzed gene expression levels in various tissues of key enzymes known to be involved in hormone synthesis. They found that androsterone, a steroid from the backdoor pathway, which can be converted to DHT, was the principal androgen in the male fetal circulation, and that levels of both androsterone and testosterone were lower in the female fetal circulation. They also found that enzymes needed for the backdoor pathway were present primarily in non-gonadal tissue, including the liver and the placenta.
Since androsterone can be made from progesterone, the authors suggest that placental progesterone or related compounds are the likely source of androsterone in the backdoor pathway. While it remains unclear why a sex difference in fetal androsterone levels exists, the authors found high expression in the male genital tubercle of enzymes required to convert androsterone to DHT. The male genital tubercle appears, therefore to be able to convert both testosterone and androsterone into DHT.
"They also suggest an explanation for why disorders of placental insufficiency can lead to hypospadias and other abnormalities of growth of the male external genitalia."
Source-Eurekalert