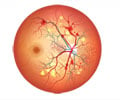
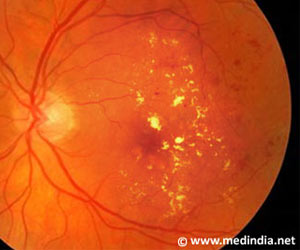
You can restore eyesight in patients with diabetic retinopathy by blocking a second blood vessel growth protein, along with one that is already well-known.

To find an explanation, researchers tested levels of VEGF in samples of fluid from the eye taken from healthy people, people with diabetes who did not have diabetic retinopathy and people with diabetic retinopathy of varying severity. While levels of VEGF tended to be higher in people with proliferative diabetic retinopathy, some of their fluid had less VEGF than did the healthy participants. But even the low-VEGF fluid from those with proliferative diabetic retinopathy stimulated blood vessel growth in lab-grown cells. Sodhi said, "The results suggested to us that although VEFG clearly plays an important role in blood vessel growth, it’s not the only factor."
A series of experiments in laboratory-grown human cells and mice revealed a second culprit, a protein called angiopoietin-like 4. When the researchers blocked the action of both VEGF and angiopoietin-like 4 in fluid from the eyes of patients with proliferative diabetic retinopathy, it markedly reduced blood vessel growth in lab-grown cells. Sodhi said, "If a drug can be found that safely blocks the second protein’s action in patients’ eyes, it might be combined with the anti-VEGF drugs to prevent many cases of proliferative diabetic retinopathy."
The research team is now investigating whether angiopoietin-like 4 might also play a role in other eye diseases, such as macular degeneration, which destroys the central portion of the retina.
Source-Medindia
 MEDINDIA
MEDINDIA


 Email
Email