A new genetic link between cardiac arrhythmias and thyroid dysfunction has been identified by Weill Cornell Medical College researchers.
A new genetic link between cardiac arrhythmias and thyroid dysfunction has been identified by Weill Cornell Medical College researchers.
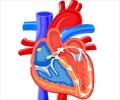
The researchers say that genes previously known to be essential to a healthy heartbeat have now also been found to play a key role in thyroid hormone (TH) biosynthesis.Writing about their findings in a paper, the researchers say that their work suggests that mutations of either of two gene products-proteins called KCNE2 and KCNQ1, which are already known to be involved in human cardiac arrhythmias-can also cause thyroid dysfunction.
"It has long been known that the thyroid influences cardiac function and cardiac arrhythmias, but our findings demonstrate a novel genetic link between inherited cardiac arrhythmia and thyroid dysfunction," Nature magazine quoted study senior author Dr. Geoffrey W. Abbott, associate professor of pharmacology in medicine at Weill Cornell Medical College, as saying.
The researchers also say that, in some cases, assessing the thyroid status of patients with KCNE2- and KCNQ1-linked cardiac arrhythmias may reveal a potential endocrine component to their cardiac arrhythmias that may not have been previously determined.
In turn, the researchers add, this may indicate treatment of the thyroid condition, with potentially beneficial effects on cardiac function.
Recognized more than a decade ago, KCNQ1 and KCNE2 are known to form potassium channels in cardiac muscle that help end each heartbeat in a timely fashion.
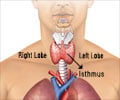
The researchers have now discovered that KCNQ1 and KCNE2 also form a potassium channel in the thyroid gland.
During the study, the researchers removed the KCNE2 gene from some mice, which, they observed, cause the animals to develop symptoms of hypothyroidism, especially during pregnancy, and gave birth to pups with dwarfism, alopecia (baldness) and cardiomegaly (enlarged heart).
In cases where the mouse pups were allowed to drink milk only from mothers without the genetic alteration, the pups' symptoms were alleviated.
The healthy mothers' milk contains normal levels of TH -- essentially acting as a TH replacement therapy. The symptoms were also treated by direct TH supplementation of pups or mothers.
"We then wanted to test what the mechanism was in the mice that caused deletion of the KCNE2 gene to have negative consequences for the thyroid," says Dr. Abbott.
He and his colleagues also used micro positron emission tomography (microPET) to visualise the accumulation in the mouse thyroid of an iodine radioisotope in real-time, and found that absorption of the radioisotope in the thyroid was greatly impaired in mice lacking the KCNE2 gene.
The researchers believe that, normally, the KCNQ1-KCNE2 potassium channel helps another protein (the sodium/iodide symporter) to transport iodide into the thyroid.
Without the KCNQ1-KCNE2 potassium channel, the efficiency of iodide absorption by the thyroid is greatly reduced. Because iodide is an essential component of TH, this means that KCNE2 deletion also impairs TH production.
Dr. Abbott has revealed that his team will next try to determing how applicable their findings in the mouse are to the human population.
"While we have identified KCNQ1 and KCNE2 in both mouse and human thyroid, much additional work is required before we can fully understand how inherited mutations in the genes coding these proteins affect human thyroid function, how this in turn influences the health of human heart and other tissues, and how useful our discoveries will be in developing therapies to treat thyroid and thyroid-related human disease," says Dr. Abbott.
A research article on the study has been published in the journal Nature Medicine.
Source-ANI
RAS
 MEDINDIA
MEDINDIA



 Email
Email