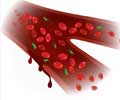
The pathogen-capturing agent, FcMBL, binds all types of living and dead infectious microbes, including bacteria, fungi, viruses, as well as toxins they release.
"The inflammatory cascade that leads to sepsis is triggered by pathogens, and specifically by the toxins they release. Thus, the most effective strategy is to treat with the best antibiotics you can muster, while also removing the toxins and remaining pathogens from the patient's blood as quickly as possible," said Wyss Institute Founding Director Donald Ingber, M.D., Ph.D., who leads the Wyss team developing the device and is the Judah Folkman Professor of Vascular Biology at Boston Children's Hospital and Harvard Medical School and Professor of Bioengineering at the Harvard John A. Paulson School of Engineering and Applied Science.
The research team's blood-cleansing approach can be administered quickly. This is because it uses the pathogen-capturing agent, FcMBL that binds all types of living and dead infectious microbes, including bacteria, fungi, viruses, as well as toxins they release.
FcMBL is a genetically engineered blood protein inspired by a naturally-occurring human molecule, which is found in the innate immune system and binds to toxic invaders, marking them for capture by immune cells in the spleen.
The new device uses the FcMBL protein to bind to all different kinds of live or dead pathogens and toxins. The optimized system uses hollow fiber filters found in regulator- approved dialysis cartridges whose inner walls are coated with FcMBL protein to remove pathogens from circulating blood. According to the researchers, in animal studies, treatment with this new pathogen-extracting device reduced the number of E. coli, Staphylococcus aureus and endotoxins circulating in the bloodstream by more than 99 percent.
Advertisement