New data presented at the Annual Congress of the European League Against Rheumatism, EULAR 2013, shows that novel antibody biomarkers could significantly improve diagnosis in rheumatoid arthritis (RA).
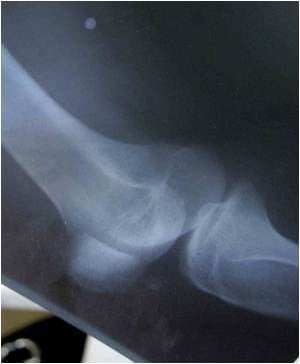
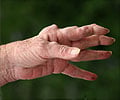
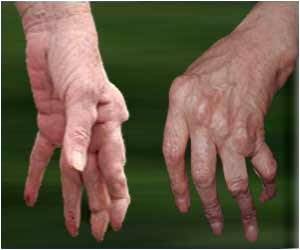
RA is a chronic autoimmune disease characterised by inflammation of the joints and tendons. As the disease progresses it can cause pain, stiffness, joint destruction and deformity, and reduce quality of life, life expectancy and physical function.
"Early detection is imperative; if treated early, patients have a more than 50% chance of achieving remission3 – yet one third of patients test negative to RF and ACCP. Antibody reactivity against our candidate biomarkers in both early and seronegative RA patients implies that they could significantly help to improve diagnosis and patient outcomes," said lead author of the study Liesbeth M De Winter, Biomedical Research Institute, Hasselt University, Diepenbeek, Belgium.
Antibody reactivity was measured in a cohort of 127 RA patients, 97 healthy controls, 90 rheumatic controls (including psoriatic arthritis, ankylosing spondylitis, osteoarthritis and Sjögren's syndrome patients) and a validation cohort of 165 RA patients. Amongst the 292 RA patients, 34% could not be identified using the current diagnostic biomarkers RF and ACCP.
"These data show that our candidates, in combination with existing biomarkers, could help close the diagnostic gap in RA. In addition, significant associations with inflammatory factors and the presence of erosions indicate a tangible prognostic potential," De Winter concluded.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email










