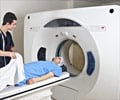
New protocol was developed for identifying neonatal patients with bronchopulmonary dysplasia by the use of magnetic resonance imaging (MRI).
TOP INSIGHT
Image-based phenotyping of neonates who are at high risk or have developed bronchopulmonary dysplasia at the time of birth could aid in early detection and timely management of the disease.
Read More..
"Up until now it has only been possible to diagnose according to clinical criteria that only allow for a low degree of differentiation ," reports Dr. Anne Hilgendorff, head of the working group "Mechanisms of Neonatal Chronic Lung Disease" at the Institute of Lung Biology (ILBD) and the Comprehensive Pneumology Center (CPC) at the Helmholtz Zentrum München and Director of the Center for Comprehensive Developmental Care (CDeCLMU) providing care for high-risk preterm and term neonates at Munich University Hospital (LMU).
Dr. Hilgendorff: "Up to now there has been a lack of specific options for assessing structural changes in the lungs while avoiding the harmful effects of radiation, and this has made personalized treatment and follow-up monitoring more difficult." A new MRT protocol could now close this gap.
Study involving 61 at-risk patients
"With our team of scientists2 in closest collaboration with our clinical colleagues in the Perinatal Center at the LMU and the Department of Radiology we have evaluated the imaging studies of 61 neonates," reports Dr. Kai Förster, a physician-scientist in Dr. Hilgendorff's working group.
Statistical analysis of the MRI data performed by colleagues from the Institute for Computational Biology at the Helmholtz Zentrum revealed increased T2 and decreased T1 relaxation times3, indicating the presence of Bronchopulmonary Dysplasia.
"In future, individual treatment and monitoring strategies will thus be possible." It is important, she stresses, that large perinatal centers now use this method and evaluate it jointly aiming at identifying potential subtypes of Bronchopulmonary Dysplasia.
Source-Eurekalert
 MEDINDIA
MEDINDIA
 Email
Email