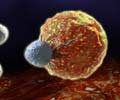
‘S1P makes cancer cells survive better by impairing the ability of T cells to target the tumor cells. Targeting S1P can decrease cancer cell survival and promote T cell activity.’
Read More..Tweet it Now
Three different signaling pathways are known to be important for regulating T cell function: the cytokine interleukin-15 (IL-15) promotes a central memory-like T cell (Tcm) phenotype that can kill unwanted cells, transforming growth factor beta (TGF-?) pushes T cells to differentiate into T regulatory cells (Tregs), and peroxisome proliferator-activated receptor gamma (PPAR?) regulates lipid metabolism, which is important for providing energy to T cells. The mechanism by which these pathways determine T cell function, however, remains unknown. Read More..
"A lot of information is known about SphK1 in tumors, but there is little known about how SphK1 regulates T cell function," says Shikhar Mehrotra, Ph.D., co-senior author, Hollings Cancer Center (HCC) researcher, associate director of the Cell Therapy Unit, and associate professor at MUSC.
To evaluate the impact of SphK1 on T cells, SphK1 function was inhibited both genetically and by using a chemical drug. They found that inhibition of SphK1, and therefore reduced S1P levels, led to a Tcm phenotype that reduced tumor size and decreased mortality in preclinical cancer models.
"When we inhibit S1P, generated by SphK1, we can make these T cells more active for killing tumors," says Besim Ogretmen, Ph.D., co-senior author, HCC researcher, program coleader of HCC's Developmental Cancer Therapeutics Research Program, professor and SmartState endowed chair of biochemistry and molecular biology at MUSC. "I think this was the first discovery that internal lipid signaling can play an important role in regulating the function of T cells against cancer cells."
They next worked out the mechanism of how SphK1 influences the T cell phenotype. Depletion of S1P levels increased the activity of a transcription factor that turns on genes associated with the memory phenotype. Additionally, loss of S1P reduced the activity of PPAR?, with two consequences: reduced PPAR? activity prevented T cells from differentiating into Tregs, and reduced PPAR? activity led to an increase in lipid utilization for energy production. Cumulatively, the multiple impacts of S1P depletion led to the Tcm phenotype.
Advertisement
These molecular details explain the different impacts of T cell regulation that were known previously. IL-15 leads to a Tcm phenotype by inhibiting SphK1 and S1P; conversely, TGF-? pushes cells towards the Treg phenotype by activating SphK1. Furthermore, these different pathways influence each other to intricately control T cell fate.
Advertisement
Common cancer treatments often center around chemotherapy, which not only targets and kills cancer cells but also kills immune cells. Targeting SphK1 allows the immune cells to stick around to target and kill cancer cells. Furthermore, Mehrotra and Ogretmen have shown that combination therapy, using a drug called PD1 mixed with compounds that inhibit SphK1, increased the efficacy of treatment in preclinical models.
"There is a lot of communication between the cancer cells in the body and the immune cells," says Ogretmen. "We don't really understand this communication yet and whether the cancer cells signal to the T cells to increase their S1P levels, making them more inactive."
Interestingly, S1P levels are high in cancer cells, allowing them to survive better. This might also impact the ability of T cells to target the cancer cells. This new work suggests that depletion of S1P might function in two ways, both inhibiting cancer cell survival and promoting T cell activity.
"This has opened up many interesting areas of further research," says Mehrotra. "Now we know that just by modulating intrinsic levels of S1P you can reach a different phenotype."
"The key is understanding the mechanism of how this pathway regulates T cell function and differentiation," adds Ogretmen.
This work paves the way to calibrate T cell immunotherapy for cancer by dampening the accumulation of S1P. Future work will be aimed at validating this pathway in several preclinical cancer models. While the mechanism of action should not change across the various model systems, this is an important next step in bringing this therapy to the clinic. Furthermore, Mehrotra and Ogretmen think this pathway has the potential to modulate autoimmune diseases such as multiple sclerosis, lupus and colitis.
Source-Eurekalert