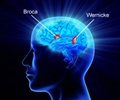
One-third of patients suffer depression following a stroke, finds recent study.

Mental disorders are common after stroke. They include anxiety, irritability and agitation, uncontrollable crying, apathy, delusions and hallucinations. But the most common disorder is depression, either major or minor.
Some patients recover over time, while others move in and out of depression. For some patients, depression doesn't develop until up to two years after the stroke.
Post-stroke depression (PSD) is linked to worse functional outcomes and increased risks of suicide and mortality.
Women are more likely to suffer PSD. Other risk factors include living alone and away from family members, higher levels of education, changes in lifestyle or marital status and degree of functional impairment. Depression, in turn, is a risk factor for stroke and stroke recurrence, even after controlling for other risk factors.
Given the severe effects of PSD, doctors should take an aggressive approach. Timing of medication may be crucial, with early treatment perhaps advantageous.
"Taken together, the available data make a strong case for the prophylactic use and effectiveness of antidepressants post stoke," the researchers said.
Source-ANI
 MEDINDIA
MEDINDIA



 Email
Email