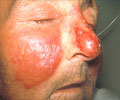
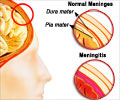
A major cause of serious infectious diseases including sepsis, meningitis and pneumonia is the Group B streptococcus.
Passed from mother to child during birth, group B streptococcus is the most common cause of infection in newborns. Guidelines for the prevention of disease have been widely adopted in high-income countries. But despite these efforts, the bacterium remains a leading cause of blood stream infections and meningitis worldwide, typically affecting babies younger than 7 days (early-onset) or infants up to 3 months of age (late-onset).
In many European countries, including the Netherlands, antibiotic treatment to prevent neonatal group B streptococcal disease is only offered to pregnant women with known risk factors for perinatal disease.
Using nationwide surveillance data from 1987 to 2011, a team of Dutch researchers examined group B streptococcus disease trends before and after the introduction of these guidelines in the Netherlands in 1999. The analysis revealed that the incidence of early-onset disease increased from 0.11 to 0.19 cases per 1000 livebirths between 1987 and 2011, and the incidence of late-onset disease increased from 0.03 to 0.13 livebirths.
Importantly, the authors note that the continuing increase in disease incidence after the adoption of the guidelines was mainly a result of a rise in the number of cases caused by clonal complex 17 strains of group B streptococcus.
Lead author Dr Arie van der Ende from the Reference Laboratory for Bacterial Meningitis, Amsterdam, Netherlands says, "Our findings should lead to a reassessment of current practices. Only offering antibiotic treatment during labour to pregnant women at risk is probably too limited to prevent all group B streptococcal infections in newborn infants. Moving to universal screening of pregnant women by vaginal and rectal swabs for group B streptococcus and offering antibiotic prophylaxis to group B streptococcus positive pregnant women must be considered."
Source-Eurekalert
 MEDINDIA
MEDINDIA
 Email
Email