In intensive-care units (ICUs), ventilator-associated pneumonia (VAP) is one of the most frequent healthcare-associated infections found.
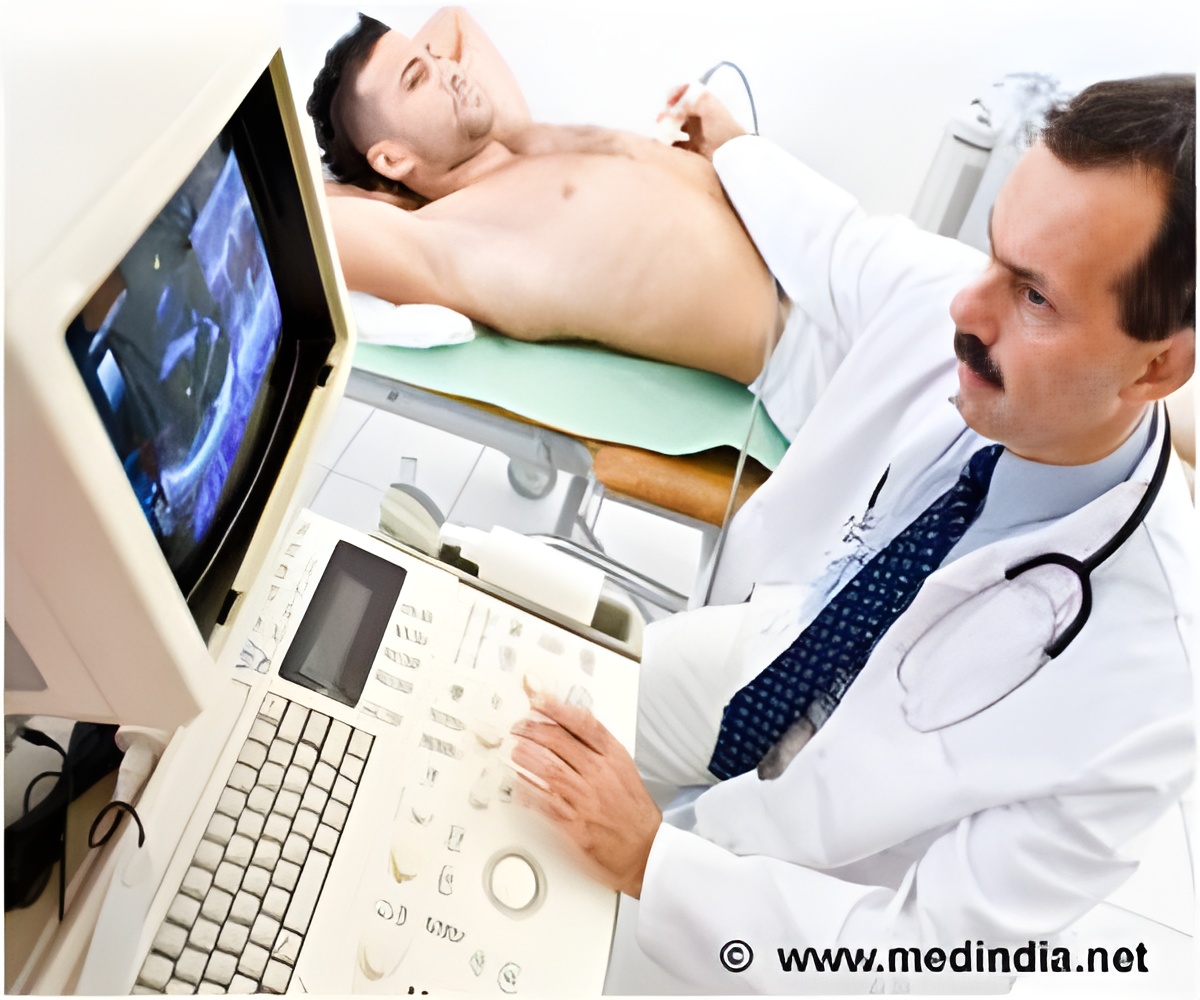
"Although it is unclear why small community hospitals experience more cases of ventilator-associated pneumonia, it may be related to limited familiarity with ventilator use and fewer specialty healthcare workers such as respiratory therapists," said Deverick Anderson, MD, MPH, an author of the study and assistant professor of medicine at Duke University and co-director of the Duke Infection Control Outreach Network.
Community hospitals are local healthcare facilities where patients generally seek short-term care and treatment. With most research on VAP focusing on large, academic medical centers such as teaching hospitals, the researchers conducted this prospective study using surveillance data to help understand the epidemiology of VAP in this healthcare setting.
The findings suggest ventilator care and outcomes are different in small community hospitals and that these hospitals may need additional resources to care for these critically ill patients. Previous research has found that VAP affects nearly 80 percent of patients intubated for longer than 24 hours and is associated with a high mortality rate and increased healthcare costs. In this study, the researchers found that patients on ventilators had long hospital stays (26 days median length of stay), and one out of three patients died.
The study reviewed a total of 247 VAP cases observed in the community hospitals over the four-year study period. These cases accounted for 192,143 ventilator-days, 504,900 ICU days and 6,763,829 patient-days. VAP infections were relatively uncommon in the study hospitals, accounting for an average of 1.4 infections per hospital each year. However, this is a higher incidence than reported nationally in 2009 by the Centers for Disease Control and Prevention's National Healthcare Safety Network for medical/surgical nonteaching hospitals (1.1.2).
"Our research may also suggest that staff at community hospitals are inexperienced with evidence-based protocols to prevent pneumonia in these under-resourced settings," said Anderson.
 MEDINDIA
MEDINDIA


 Email
Email