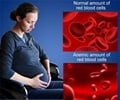
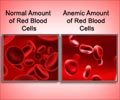
Conclusive data of a key clinical trial studying the drug's efficacy show that hydroxyurea therapy offers safe and effective disease management of sickle cell anemia (SCA).
"Early results indicate that TWiTCH is a success. Hydroxyurea works as well as blood transfusions to lower TCD velocities, which lowers the risk of the child having a stroke," said Russell E. Ware, MD, PhD, principal investigator of the study and director of Hematology at Cincinnati Children's Hospital Medical Center, which served as the study's Medical Coordinating Center.
"A group of outside experts has been reviewing the TWiTCH data every few months to ensure the safety of children in the clinical trial and to monitor the data," Ware explained. "This group met recently and after careful consideration of the interim data results, recommended that the study be stopped since hydroxyurea worked as well as transfusions to lower TCD velocities."
The NHLBI and National Institutes of Health (NIH) agreed with the recommendation. "No child should ever suffer a stroke, which is why it was so important for the NHLBI to support the TWiTCH trial," said Gary Gibbons, MD, director of the NHLBI. "This critical research finding opens the door to more treatment options for clinicians trying to prevent strokes in children living with the sickle cell disease."
The study enrolled its first patient in September 2011 and included children between ages 4 and 16 years with sickle cell anemia and abnormally elevated TCD velocities, which increases their risk of developing a stroke. The current standard therapy for children with elevated TCD velocities is monthly blood transfusions. A total of 121 children were randomized: half received the standard therapy of transfusions while the other half received the alternate treatment with daily hydroxyurea, which has not yet been approved for children with sickle cell anemia.
The clinical data-collection portion of the study was originally scheduled for 24 months, but collection is now being stopped early, after only half of the children have completed the treatment phase.
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email