The new Risk of Ovarian Cancer Algorithm (ROCA) helps in detection of ovarian cancer at an early stage especially in high-risk women.
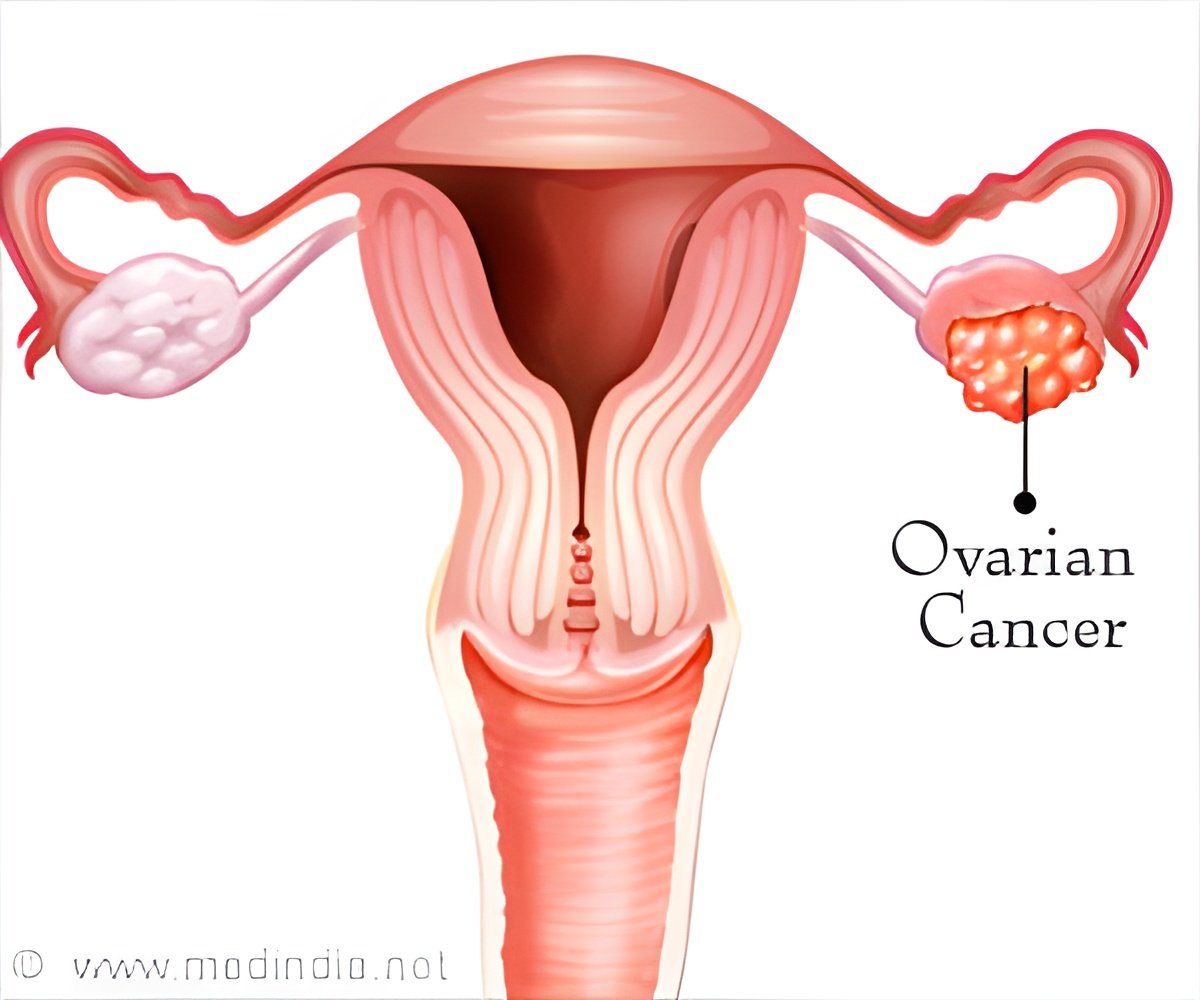
- Women who face an increased risk of ovarian cancer due to family history or genetic mutations are advised to have surgeries to get their ovaries and fallopian tubes removed.
- New trial uses the Risk of Ovarian Cancer Algorithm (ROCA) to track CA125 levels especially in women who postpone the recommended surgery.
- The levels of CA125 protein are known to be raised over 35 in the blood of most women with ovarian cancer.
- This algorithm helps to calculate the risk by tracking to CA125 levels over time to identify significant elevations above each patient's baseline levels.
TOP INSIGHT
The new screening protocol involving tracking CA125 protein levels using Risk of Ovarian Cancer Algorithm (ROCA), helps to increase the proportion of tumors detected at early stages from 10% to 50%.
"The standard advice for women at high risk of ovarian cancer, due to either family history or inherited gene mutations, is to have their ovaries and fallopian tubes removed once their families are complete. Some women choose to postpone this surgery," says Steven Skates, PhD, of the Massachusetts General Hospital (MGH) Cancer Center and the Biostatistics Unit, co-lead and corresponding author of the report.
"Our screening protocol increased the proportion of tumors detected at early stages from 10 percent - which is typically seen in high-risk women who are not screened - to 50 percent." Stakes added.
The levels of CA125 protein are known to be raised over 35 in the blood of most women with ovarian cancer.
Risk of Ovarian Cancer Algorithm (ROCA)
One trial was led by Steven Skates and conducted through the National Cancer Institute's Cancer Genetics Network (CGN). Between 2001 and 2011, the CGN trial enrolled 2,359 women at 25 U.S. sites.
In both trials, women with elevated risk for ovarian cancer based on either a strong family history of ovarian and/or breast cancer or the presence of risk-associated mutations in the BRCA1 or BRCA2 genes, who had not yet had risk-reducing surgery were recruited.
Participants had CA125 blood tests utilizing ROCA every three months. Previously, they were screened for raised CA125 values every 6 or 12 months .
A patient's ROCA risk was calculated by analyzing the results of each new CA125 test, combined with previous results and factors such as age and menopausal status. ROCA helps to calculate risk when a baseline has been established.
Women with intermediate ROCA risk were referred for an ultrasound examination, while those at an elevated ROCA risk received both ultrasound and clinical evaluation by a gynecologic oncologist.
From both the trials, 19 malignant tumors of the ovaries or fallopian tubes were identified during the study periods. Ten cases were diagnosed during screening, and nine were diagnosed by preventive surgery.
Among the 10 cases, 4 were present at the outset of the trial, while 6 tumors were likely to have developed during the trial period after a CA125 baseline had been measured.
The results in these six cases reflect the benefits of a long-term ROCA screening program. All cases except one were diagnosed by ROCA, giving a sensitivity of over 80%, and around 50% were detected at early stages.
"It is important to note that removal of ovaries and fallopian tubes remains the standard of care when women at increased familial or genetic risk complete their families and reach an age when their risk exceeds that of the general population," stresses Skates.
Mark Greene said "Surgery is the primary and best option for reducing the risk of ovarian cancer, and ROCA should only be considered as a promising but unproven option for patients who decide, against medical advice, to postpone their surgery."
Further research is needed to identify a greater range of ovarian cancer biomarkers and improved imaging technologies, to help detect more tumors at even earlier stages.
The paper is published in Clinical Cancer Research.
Reference
- Steven Skates et al. Early Detection of Ovarian Cancer using the Risk of Ovarian Cancer Algorithm with Frequent CA125 Testing in Women at Increased Familial Risk - Combined Results from Two Screening Trials. Clinical Cancer Research; (2017) DOI: 10.1158/1078-0432.CCR-15-2750
Source-Medindia
 MEDINDIA
MEDINDIA


 Email
Email










