A decline in understanding of the speech could serve as a predictor of early dementia.
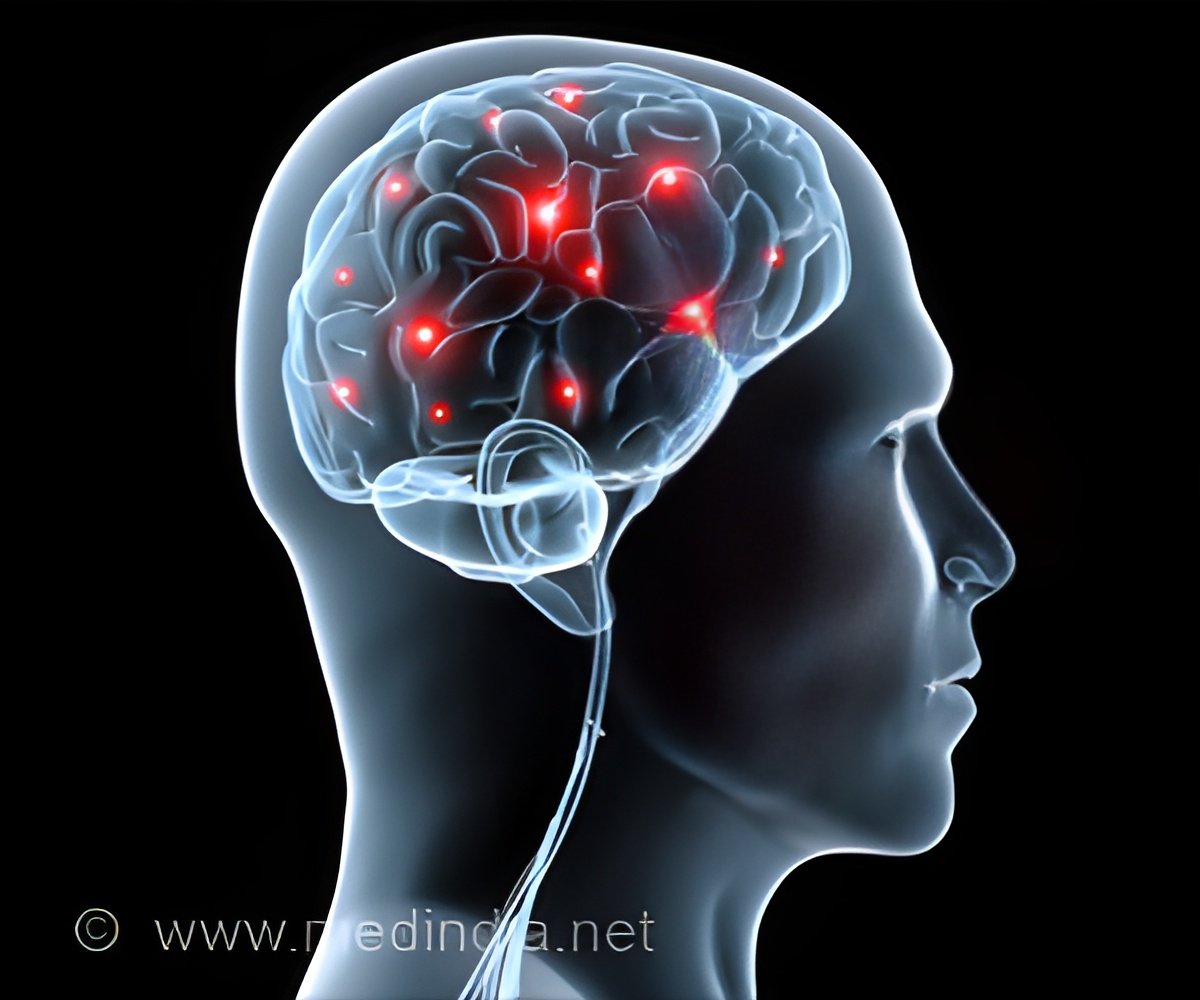
- Abnormal functionality in regions of the brain that process speech sound, the brainstem and auditory cortex, could be a new potential predictor of early dementia.
- This decline in brain function related to communication could be the first sign that manifests before the individuals become aware of these problems.
- This functional biomarker could help to identify people who should be monitored more closely for their risk of developing dementia.
TOP INSIGHT
Developing targeted treatments or interventions to maintain the ability to communicate could help to slow the progression of dementia.
The findings demonstrates that changes occur early during the brain's conversion of speech sound into understandable words.
Study
The study examined 23 older adults between the ages of 52 and 86 years with no known history of neurological or psychiatric illnesses with similar hearing acuity.
Participants were separated into two groups based on their results on a dementia screening test.
Researchers combined both sets of brain activity, using statistical methods, to predict mild cognitive impairment.
The brain activity within the brainstem of these older adults demonstrated abnormally large processing of speech sound within 7-10 milliseconds of the signal hitting the ear. This could be sign of greater communication problems in the future.
"Losing the ability to communicate is devastating and this finding could lead to the development of targeted treatments or interventions to maintain this capability and slow progression of the disease." Alain added.
"When we hear a sound, the normal aging brain keeps the sound in check during processing, but those with MCI have lost this inhibition and it was as if the flood gates were open since their neural response to the same sounds were over-exaggerated," says Dr. Gavin Bidelman, first author on the study, a former RRI post-doctoral fellow and assistant professor at the University of Memphis.
"This functional biomarker could help identify people who should be monitored more closely for their risk of developing dementia." Bidelman added.
The researchers used electroencephalogram (EEG) to measure electrical activity using in these brain regions. This technique also helped predict mild cognitive impairment (MCI), with 80% accuracy.
This test could be developed into a cost-effective and objective diagnostic assessment for older adults.
"MCI is known to cause changes in different senses, such as vision or touch," says Dr. Alain. "If we could incorporate these changes into a wireless EEG test, we could combine all this information and develop a better biomarker. One day, doctors could administer a short, 10-minute assessment and instantly provide results."
"This could offer a new diagnostic assessment that tests a person's cognitive abilities, such as their ability to communicate, and objectively measure physiological changes in the brain that reflect early signs of dementia," says Dr. Bidelman.
The study is published online in the Journal of Neuroscience.
Reference
- Claude Alain et al. Mild cognitive impairment is characterized by deficient brainstem and cortical representations of speech. Journal of Neuroscience; (2017) doi.org/10.1523/JNEUROSCI.3700-16.2017
Source-Medindia
 MEDINDIA
MEDINDIA


 Email
Email





