Homocysteine levels are not measured in most traditional screening tests, but the relationship between these levels & cardiovascular disease development has drawn greater scrutiny in recent times.

When does it pose a problem?
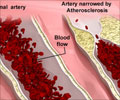
Homocysteine in itself is not a problem and is present in all healthy individuals. Under normal circumstances, homocysteine in your blood stream undergoes yet another change, being converted into cysteine or it can even be transformed back into methionine. While Vitamin B6 is necessary for the conversion to cysteine, B12 enzymes are necessary for the transformation back to methionine. Cysteine is an extremely important protein and it is necessary for various bodily functions including the metabolism of various minerals like zinc, iron and copper.When this normal processing or utility of homocysteine cannot be fulfilled and it remains in the body as is, the levels are elevated. While the co-relation between elevated homocysteine levels and cardiac disease is still not clear and widely debated, there is a clear link that higher levels of homocysteine is associated with strokes, heart attacks, hypertension, blood clot formation and arteriosclerosis.
Why does this elevation of homocysteine happen?
Although the reasons for this impaired ability to metabolise homocysteine properly are not always clear, it is often caused because of nutritional deficiencies with low levels of vitamins B6 and B12 and folic acid. Alcoholism can also contribute to the problem as malnutrition; a Vitamin B deficiency is common in alcoholics. Some experts also believe that alcohol itself may directly contribute to the homocysteine elevation, with or without any nutritional deficiencies.When do you need to get tested?
Homocysteine testing is still rather expensive as it is not a part of routine screening or diagnostics. Homocysteine levels are, in fact, only checked in certain conditions, if the concerned healthcare provider requests testing. This is often done when dealing with patients suffering from cardiac disease, strokes, heart attacks or blood clots who are still young adults. Such patients are screened for any kind of abnormalities with blood clotting and for homocysteine levels as well. Homocysteine levels are also often tested when patients without any identifiable risk factors suffer from conditions like heart attacks or strokes.What can I do about high homocysteine levels?
Your health care provider will recommend a suitable course of action if your levels are found to be high. Folic acid and vitamin supplementation to raise vitamins B6 and B12 intake are given for treating homocysteinuria, which is a condition of elevated homocysteine levels. The efficacy of such a treatment is closely monitored with regular blood tests and in some cases, it is found that patients do not respond to treatment as they may be pyridoxine-resistant. Dietary modifications to reduce the intake of methionine sources can also help. This means cutting down your intake of foods like eggs, fish, meat, certain plant seeds and cereal. At the same time, don’t forget that methionine is an essential amino acid and should not be eliminated altogether from your diet.Keep in mind that most studies do not show in decreased risk even after lowering homocysteine levels. It would appear that the risk that develops with elevated homocysteine levels does not dissipate altogether even with lowering of the levels. For this reason, it is better to avoid foods that greatly increase the risk of elevating homocysteine levels.
References:
1. Wierzbicki AS. Homocysteine and cardiovascular disease: a review of the evidence. Diab Vasc Dis Res. 2007 Jun;4(2):143-50. Review. PubMed PMID: 17654449.2. http://en.wikipedia.org/wiki/Homocysteine
Source-Medindia
 MEDINDIA
MEDINDIA



 Email
Email