Combining Magnetic Resonance Imaging (MRI) with conventional screening may greatly improve prostate cancer detection and help avoid unnecessary biopsies, show initial results from the Goteborg randomised screening trial. The trial is a Swedish version of the European Randomized Study of Screening for Prostate Cancer, which is considered to be the largest randomized prostate cancer screening trial.
In 2014, results from this trial found a significant mortality reduction with prostate-specific antigen (PSA) screening for men aged 55-69 years of age. Now, a new study presented at the European Association of Urology (EAU) Conference in Madrid (going on till 24 March 2015) shows that using MRI may further improve the accuracy of prostate cancer screening.The experiment has been awarded the EAU’s First Prize for the Best Abstract by a Resident.
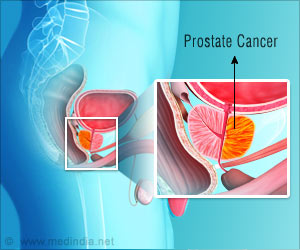
Prostate cancer is the second most common cancer in men after lung cancer and second leading cause of cancer death in men in Western Europe. More than 670,000 men are diagnosed with prostate cancer every year worldwide.
In many cases, screening for prostate cancer using Prostate-specific antigen (PSA) tends to give false negatives and false positives. Hence, many men are subject to invasive testing and perhaps treatment, which was just not necessary.
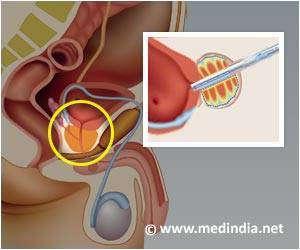
Prof.Jonas Hugosson and his Swedish research team chose 384 patients attending the Goteborg trial, and asked 124 of them to go for an MRI prior to having a biopsy. Those with a suspicious MRI, or with a PSA > 3 ng/ml, were recommended for biopsy. Tissue samples taken at random from the prostate are called standard samples and samples from the suspicious areas seen on the MRI are targeted samples. Scientists took standard and targeted samples.
The experiment found that the combining PSA and MRI gave better prostate cancer. The results also showed that even potentially aggressive cancers were detected with PSA, MRI combination screening compared with using PSA stand-alone test in screening.
“From these initial results, it looks like we can combine PSA levels with MRI scans to give more accurate screening results. This strategy would allow us to take men with lower PSA scores, and give them MRI scans, to confirm whether or not a biopsy is absolutely necessary,” said Dr.Anna Grenabo-Bergdahl, Sahlgrenska University Hospital, Goteborg, Sweden. “Another benefit is that the MRI helps us locate the suspect area, meaning that if we have to do a confirmatory biopsy, we have a much better idea of where the problem might be. This avoids patient stress, and means we are less likely to miss cancers.”
Prof.Manfred Wirth, EAU Treasurer, concurred, and said, “We definitely need a bigger research to validate these results. There are some real issues to address. For example, MRI is currently not cost-effective to use in routine screening and we cannot consider it for routine screening as well.”