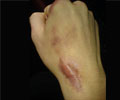
Whether diabetic foot wounds heal or worsen depends on first, how patients cope with these ulcers, and second, their levels of depression, claims a University of Nottingham study.

The study has sparked a follow-on project to develop psychological treatments to reduce depression in sufferers and help them cope more effectively with this debilitating and potentially life-threatening condition.
Foot ulcers are open sores which form when a minor skin injury fails to heal because of microvascular and metabolic dysfunction caused by diabetes.
Up to fifteen per cent of people with diabetes, both Type 1 and Type 2, develop foot or leg ulcers with many suffering depression and poorer quality of life as a result.
During the five-year study 93 patients (68 men and 25 women) with diabetic foot ulcers were recruited from specialist podiatry clinics across the UK. Clinical and demographic determinants of healing; psychological distress, coping style and levels of cortisol (a stress hormone) in saliva were assessed and recorded at the start of a 24 week monitoring period.
The size of each patient's ulcer was also measured at the start, and then at 6, 12 and 24 weeks to record the extent of healing or otherwise of the ulcer.
Surprisingly perhaps, patients who showed a 'confrontational' way of coping (a style characterised by a desire to take control) with the ulcer and its treatment were less likely to have a healed ulcer at the end of the 24 week period.
A secondary analysis of each patient examined the relationship of psycho-social factors with the change in the size of the ulcer over the observation period.
Whereas the first analysis showed that only confrontation coping, not anxiety or depression, was a significant predictor of healing, the second showed that depression was a significant predictor in how the size of the ulcer changed over time, with patients with clinical depression showing smaller changes in ulcer size over time i.e., they showed less improvement or healing.
The study is published in the journal Diabetologia this month.
Source-ANI
 MEDINDIA
MEDINDIA



 Email
Email