Women with certain types of human leukocyte antigen (HLA) may have an increased risk of ovarian cancer and may also respond better to immunotherapy.
TOP INSIGHT
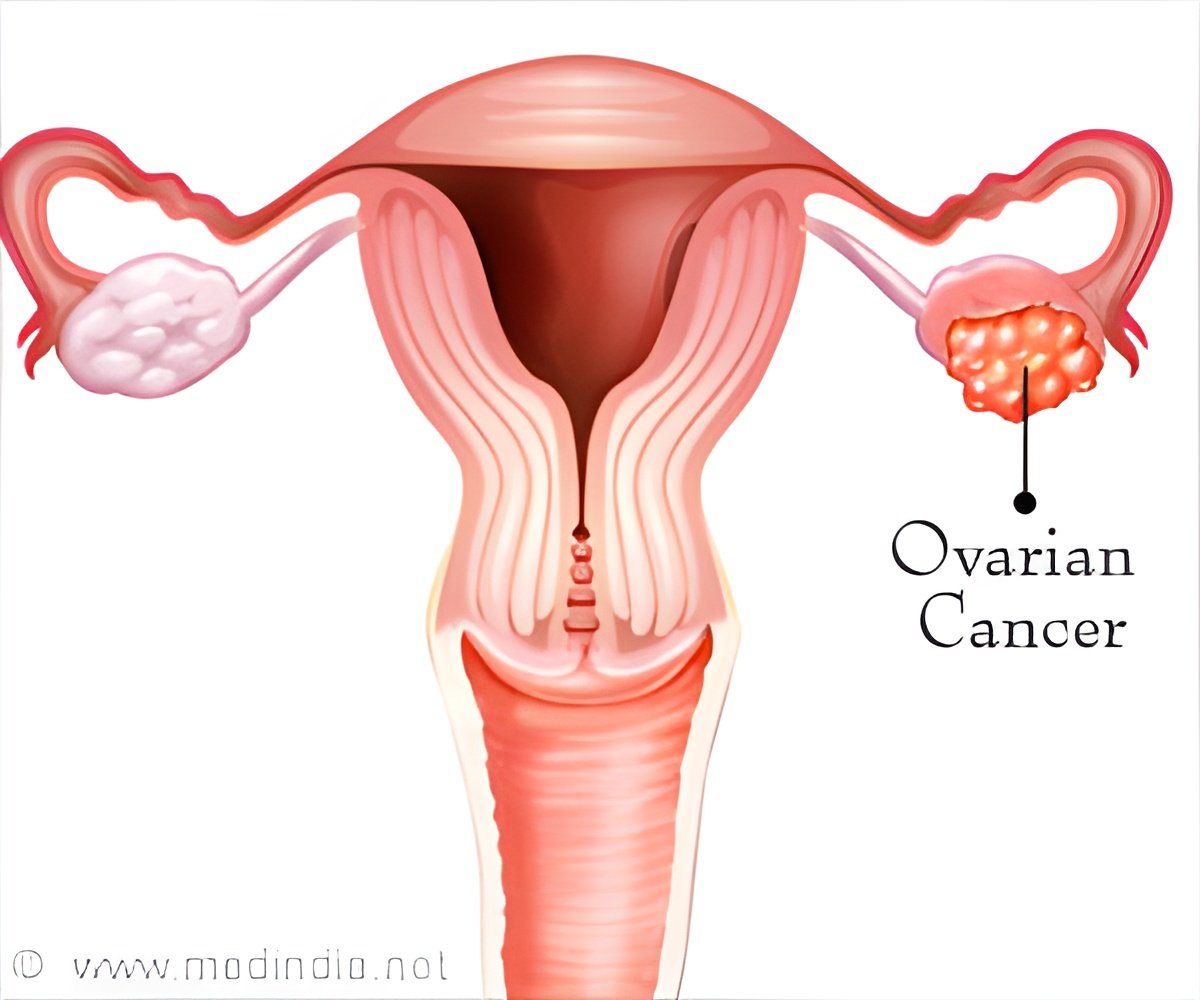
Women with certain types of human leukocyte antigen (HLA) may have an increased risk of ovarian cancer and may also respond better to immunotherapy.
Kunle Odunsi, senior author of the study, who is Deputy Director, M. Steven Piver Professor and Chair of the Department of Gynecologic Oncology and Executive Director of the Center of Immunotherapy at Roswell Park, said, "Immunotherapy has emerged as a promising and powerful tool in the fight against ovarian cancer. This research offers important insights into how to understand and employ the immune system to more effectively fight this disease."
Researchers identified 126 patients at Roswell Park who underwent HLA testing to determine their eligibility for several clinical trials between January 2002 and December 2012. This study was designed to determine whether HLA subtypes differ between ovarian cancer patients with or without spontaneous immune response to NY-ESO-1, a protein expressed in cancers but not in normal tissue. The two major findings were that patients with the B27 HLA subtype were more likely than the general population to be diagnosed with ovarian cancer and that the B44 subtype had a worse prognosis.
"The clinical significance of an association between specific HLA subtypes and the risk of developing ovarian cancer cannot be overstated, as this may represent a new population of patients at risk for the disease. Larger studies are needed to evaluate the potential impact of these results," adds the study's lead author, J. Brian Szender, Department of Gynecologic Oncology at RPCI.
Source-Newswise
 MEDINDIA
MEDINDIA



 Email
Email










