Patients with obstructive sleep apnea face an elevated risk of perioperative complications; the risk is higher if the diagnosis has not been made before surgery.
Obstructive sleep apnea (OSA) consists of brief respiratory pauses arising repeatedly in a particular period of time while the patient sleeps. At least one in five adults about to undergo surgery suffers from OSA.
Patients with OSA face an elevated risk of perioperative complications; the risk is even higher if the diagnosis has not been made before surgery. This is so for many OSA patients, as Philipp Fassbender and colleagues point out in a review in the current issue of
Deutsches International.
TOP INSIGHT
Patients with obstructive sleep apnea (OSA) face an elevated risk of perioperative complications; the risk is higher if the diagnosis has not been made before surgery.
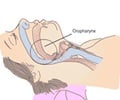
In patients requiring surgery, sedation and anesthesia weaken the activation of the airway-opening muscles just as sleep does, potentially leading to airway obstruction. This elevates the risk of perioperative complications - e.g., because of difficult intubation - in patients with OSA. Thus, as the authors stress, it is important for OSA patients to be identified before surgery, so that the anesthesia technique can be modified accordingly.
The special features of OSA patients and the complications for which they are at elevated risk call for expertise and meticulous attention on the anesthesiologist's part. Local and regional anesthesia are preferable to general anesthesia for such patients. If deeper sedation is needed, the potential effect on the airways must be borne in mind.
Source-Eurekalert

 MEDINDIA
MEDINDIA

 Email
Email










