Children and adolescents with seizures involving the temporal lobe are likely to have clinically significant behavioral problems and psychiatric illness, especially depression, determined a new study.
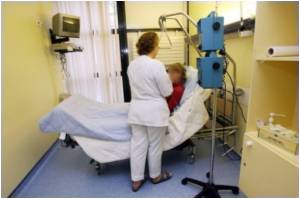
Current medical evidence indicates that mental illness occurs in up to 40% of pediatric epilepsy patients, with depression, anxiety, attention issues and learning difficulties being the most common psychiatric conditions in children. Furthermore, a 2009 study of adult surgical patients found that depression was associated with seizures in the temporal lobe—a common focus for surgically treated epilepsy according to Sanchez-Gistau et al.1 However, such evidence is not well established in pediatric patients and is the focus of the present study.
"Our research examined whether psychiatric illness was more prominent in children who were unresponsive to anti-seizure medications and had seizures in the temporal lobe versus elsewhere in the brain," explains lead study author, Dr. Jay Salpekar with Children's National Medical Center in Washington, D.C. "In children who do not respond to drug therapy, epilepsy surgery may be the only option to improve their quality of life. Understanding the pediatric patients' mental health status is important, as the severity of psychiatric illness may impact the overall risk-benefit of epilepsy surgery."
For the current study, researchers reviewed case records for 40 children between the ages of 6 and 17, who did not respond to anti-seizure medications. Patients were given pre-surgical psychiatric evaluations and their parents completed the Child Behavioral Checklist (CBCL). The seizure location and suitability for surgical procedures were confirmed by epilepsy specialists.
The investigators found that this pediatric patient group had psychiatric and behavioral problems well beyond what is typically reported in children with chronic epilepsy. Nearly 80% of participants had significant psychiatric symptoms—far greater than the 20%-40% prevalence of mental illness generally found in chronic pediatric epilepsy. Furthermore, children with seizures suspected to be localized in the temporal lobe were more likely to have depression symptoms and more significant behavioral issues reported by parents compared to children with seizures in other brain regions.
Dr. Salpekar concludes, "Given that psychiatric illness, particularly depression, is so prominent in those with temporal lobe seizures, routine psychiatric evaluation appears to be important not only for adults, but also for children and adolescents prior to epilepsy surgery. In fact, it may be beneficial for most patients with medically refractory epilepsy to have a psychiatric assessment, regardless of seizure localization, to improve quality of life." Future studies are needed to investigate the variables associated with mental illness outcomes in patients following epilepsy surgery.
 MEDINDIA
MEDINDIA



 Email
Email










