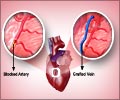
The risk of death is same in patients that received newer drug-coated stents, which keep blocked coronary arteries open, and also in those that underwent bypass surgery.

Researchers found that the stent group fared better in the first 30 days, with only half the number of deaths and one-sixth the number of strokes seen in the bypass group. But in contrast to previous studies, the stent group did not seem to fare worse in the longer term. During the period from 30 days to about 3 years on average, the numbers of deaths in the two groups were not significantly different. Patients in the stent group got about 1.5 times the number of heart attacks long-term, compared to the bypass group. But, patients whose stents successfully opened all of their diseased arteries, there was no significant increase in heart attacks.
Dr. Sripal Bangalore, an associate professor in NYU Langone’s Leon H. Charney Division of Cardiology, Department of Medicine, who was lead author of the study, said, "The key finding is that there was no greater mortality in the sample of patients receiving the latest generation stents. The gap in apparent mortality risk between bypass and PCI has been getting smaller and smaller as stent technologies have advanced."
The study was published in the New England Journal of Medicine.
Source-Newswise
 MEDINDIA
MEDINDIA
 Email
Email