Drugs, which are commonly prescribed for nausea and vomiting leads to one-third increase in the risk of potentially deadly blood clots, according to a Brit study.

Researchers said the drugs should be used more cautiously after findings from a study of more than 100,000 people found they were associated with an increased risk of blood clots. he use of antipsychotics is controversial as evidence that they are effective is limited and charities have warned they are used as a ’chemical cosh’ to subdue difficult elderly patients with dementia.
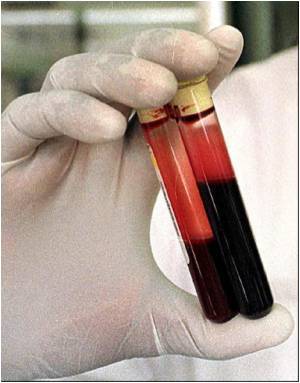
For the study, researchers at University of Nottingham investigated around 25,000 people who had suffered a blood clot, either in the legs or in the lung, and compared them with similar people who had not suffered one.
They found around three quarters of the people studied had taken prochlorperazine which is widely used to treat vertigo, nausea and vomiting.
It is not effective at treating travel or motion sickness.
The results showed that those prescribed antipsychotics in the previous two years were 32 per cent more likely to have had a blood clot.
Advertisement
People who had started taking the drugs in the previous three months were at even higher risk of clots, and were twice as likely to have had one than those not on the drugs.
Advertisement
"Though these findings add to the accumulating evidence of adverse health events associated with antipsychotic drugs, they should be confirmed with other data sources," the Telegraph quoted lead author Professor Julia Hippisley-Cox at the University of Nottingham, as saying.
"If other studies replicate these findings, antipsychotic drugs should be used more cautiously for nausea and agitation etc, especially among patients at high risk of thromboembolism.
"Patients need information on the balance of risks and benefits of these drugs before they start treatment," he added.
The findings were published online in the British Medical Journal.
Source-ANI